Related Research Articles

In mammals and other animals, the vagina is the elastic, muscular reproductive organ of the female genital tract. In humans, it extends from the vestibule to the cervix. The outer vaginal opening is normally partly covered by a thin layer of mucosal tissue called the hymen. At the deep end, the cervix bulges into the vagina. The vagina allows for copulation and birth. It also channels menstrual flow, which occurs in humans and closely related primates as part of the menstrual cycle.
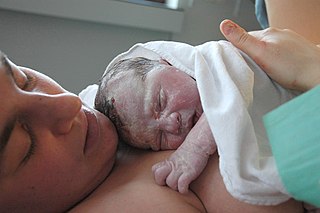
Childbirth, also known as labour, parturition and delivery, is the completion of pregnancy where one or more babies exits the internal environment of the mother via vaginal delivery or caesarean section. In 2019, there were about 140.11 million human births globally. In the developed countries, most deliveries occur in hospitals, while in the developing countries most are home births.

The perineum in mammals is the space between the anus and the genitals. The human perineum is between the anus and scrotum in the male or between the anus and vulva in the female. The perineum is the region of the body between the pubic symphysis and the coccyx, including the perineal body and surrounding structures. The perineal raphe is visible and pronounced to varying degrees. The perineum is an erogenous zone. This area is also known as the taint or gooch in American slang.

Episiotomy, also known as perineotomy, is a surgical incision of the perineum and the posterior vaginal wall generally done by an obstetrician. This is usually performed during the second stage of labor to quickly enlarge the aperture, allowing the baby to pass through. The incision, which can be done from the posterior midline of the vulva straight toward the anus or at an angle to the right or left, is performed under local anesthetic, and is sutured after delivery.

The postpartum period begins after childbirth and is typically considered to last for six weeks. There are three distinct phases of the postnatal period; the acute phase, lasting for six to twelve hours after birth; the subacute phase, lasting six weeks; and the delayed phase, lasting up to six months. During the delayed phase, some changes to the genitourinary system take much longer to resolve and may result in conditions such as urinary incontinence. The World Health Organization (WHO) describes the postnatal period as the most critical and yet the most neglected phase in the lives of mothers and babies; most maternal and newborn deaths occur during this period.
Gender-affirming surgery for male-to-female transgender women or transfeminine non-binary people describes a variety of surgical procedures that alter the body to provide physical traits more comfortable and affirming to an individual's gender identity and overall functioning.
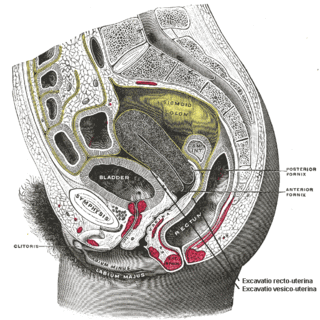
In gynecology, a rectocele or posterior vaginal wall prolapse results when the rectum bulges (herniates) into the vagina. Two common causes of this defect are childbirth and hysterectomy. Rectocele also tends to occur with other forms of pelvic organ prolapse, such as enterocele, sigmoidocele and cystocele.
Vaginoplasty is any surgical procedure that results in the construction or reconstruction of the vagina. It is a type of genitoplasty. Pelvic organ prolapse is often treated with one or more surgeries to repair the vagina. Sometimes a vaginoplasty is needed following the treatment or removal of malignant growths or abscesses to restore a normal vaginal structure and function. Surgery to the vagina is done to correct congenital defects to the vagina, urethra and rectum. It may correct protrusion of the urinary bladder into the vagina (cystocele) and protrusion of the rectum (rectocele) into the vagina. Often, a vaginoplasty is performed to repair the vagina and its attached structures due to trauma or injury.

The cystocele, also known as a prolapsed bladder, is a medical condition in which a woman's bladder bulges into her vagina. Some may have no symptoms. Others may have trouble starting urination, urinary incontinence, or frequent urination. Complications may include recurrent urinary tract infections and urinary retention. Cystocele and a prolapsed urethra often occur together and is called a cystourethrocele. Cystocele can negatively affect quality of life.

Labiaplasty is a plastic surgery procedure for creating or altering the labia minora and the labia majora, the folds of skin of the human vulva. It is a type of vulvoplasty. There are two main categories of women seeking cosmetic genital surgery: those with conditions such as intersex, and those with no underlying condition who experience physical discomfort or wish to alter the appearance of their vulvas because they believe they do not fall within a normal range.

A pelvic examination is the physical examination of the external and internal female pelvic organs. It is frequently used in gynecology for the evaluation of symptoms affecting the female reproductive and urinary tract, such as pain, bleeding, discharge, urinary incontinence, or trauma. It can also be used to assess a woman's anatomy in preparation for procedures. The exam can be done awake in the clinic and emergency department, or under anesthesia in the operating room. The most commonly performed components of the exam are 1) the external exam, to evaluate the vulva 2) the internal exam with palpation to examine the uterus, ovaries, and structures adjacent to the uterus (adnexae) and 3) the internal exam using a speculum to visualize the vaginal walls and cervix. During the pelvic exam, sample of cells and fluids may be collected to screen for sexually transmitted infections or cancer.

Clitoral hood reduction, also termed clitoral hoodectomy, clitoral unhooding, clitoridotomy, or (partial) hoodectomy, is a plastic surgery procedure for reducing the size and the area of the clitoral hood in order to further expose the glans of the clitoris.

Perineoplasty denotes the plastic surgery procedures used to correct clinical conditions of the vagina and the anus. Among the vagino-anal conditions resolved by perineoplasty are vaginal looseness, vaginal itching, damaged perineum, fecal incontinence, genital warts, dyspareunia, vaginal stenosis, vaginismus, vulvar vestibulitis, and decreased sexual sensation. Depending upon the vagino-anal condition to be treated, there are two variants of the perineoplasty procedure: the first, to tighten the perineal muscles and the vagina; the second, to loosen the perineal muscles.

A perineal tear is a laceration of the skin and other soft tissue structures which, in women, separate the vagina from the anus. Perineal tears mainly occur in women as a result of vaginal childbirth, which strains the perineum. It is the most common form of obstetric injury. Tears vary widely in severity. The majority are superficial and may require no treatment, but severe tears can cause significant bleeding, long-term pain or dysfunction. A perineal tear is distinct from an episiotomy, in which the perineum is intentionally incised to facilitate delivery. Episiotomy, a very rapid birth, or large fetal size can lead to more severe tears which may require surgical intervention.

Pain management during childbirth is the partial treatment and a way of reducing any pain that a woman may experience during labor and delivery. The amount of pain a woman feels during labor depends partly on the size and position of her baby, the size of her pelvis, her emotions, the strength of the contractions, and her outlook. Tension increases pain during labor. Virtually all women worry about how they will cope with the pain of labor and delivery. Childbirth is different for each woman and predicting the amount of pain experienced during birth and delivery can not be certain.
The postpartum physiological changes are those expected changes that occur in the woman's body after childbirth, in the postpartum period. These changes mark the beginning of the return of pre-pregnancy physiology and of breastfeeding. Most of the time these postnatal changes are normal and can be managed with medication and comfort measures, but in a few situations complications may develop. Postpartum physiological changes may be different for women delivering by cesarean section. Other postpartum changes, may indicate developing complications such as, postpartum bleeding, engorged breasts, postpartum infections.
Abuse during childbirth is generally defined as interactions or conditions deemed humiliating or undignified by local consensus and interactions or conditions experienced as or intended to be humiliating or undignifying. Bowser and Hill's 2010 landscape analysis defined seven categories of abusive or disrespectful care, including physical abuse, non-consented clinical care, non-confidential care, non-dignified care, discrimination, abandonment, and detention in health facilities.
Vaginal trauma is injury to the vagina. It can happen during childbirth, sexual assault, and accidental occurrences.

Vaginal cysts are uncommon benign cysts that develop in the vaginal wall. The type of epithelial tissue lining a cyst is used to classify these growths. They can be congenital. They can present in childhood and adulthood. The most common type is the squamous inclusion cyst. It develops within vaginal tissue present at the site of an episiotomy or other vaginal surgical sites. In most instances they do not cause symptoms and present with few or no complications. A vaginal cyst can develop on the surface of the vaginal epithelium or in deeper layers. Often, they are found by the woman herself and as an incidental finding during a routine pelvic examination. Vaginal cysts can mimic other structures that protrude from the vagina such as a rectocele and cystocele. Some cysts can be distinguished visually but most will need a biopsy to determine the type. Vaginal cysts can vary in size and can grow as large as 7 cm. Other cysts can be present on the vaginal wall though mostly these can be differentiated. Vaginal cysts can often be palpated (felt) by a clinician. Vaginal cysts are one type of vaginal mass, others include cancers and tumors. The prevalence of vaginal cysts is uncertain since many go unreported but it is estimated that 1 out of 200 women have a vaginal cyst. Vaginal cysts may initially be discovered during pregnancy and childbirth. These are then treated to provide an unobstructed delivery of the infant. Growths that originate from the urethra and other tissue can present as cysts of the vagina.
Vaginal stenosis is an abnormal condition in which the vagina becomes narrower and shorter due to the formation of fibrous tissue. Vaginal stenosis can contribute to sexual dysfunction, dyspareunia and make pelvic exams difficult and painful. The lining of the vagina may also be thinner and drier and contain scar tissue. This condition can result in pain during sexual intercourse or a pelvic exam. Vaginal stenosis is often caused by radiation therapy to the pelvis, an episiotomy, or other forms of surgical procedures. Chemotherapy can also increase the likelihood of developing vaginal stenosis. Vaginal stenosis can also result from genital reconstructive surgery in people with congenital adrenal hyperplasia.
References
- ↑ Kitzinger, Sheila (1994). The Year After Childbirth (1st ed.). Oxford: Oxford University Press. p. 71. ISBN 978-0192177841.
- 1 2 3 4 Vinopal, Lauren (17 August 2017). "Who's Afraid of the 'Husband Stitch'? New Moms Everywhere". Fatherly. Archived from the original on 16 October 2017. Retrieved 15 October 2017.
- 1 2 Dobbeleir, Julie M. L. C. L.; Van Landuyt, Koenraad; Monstrey, Stan J. (May 2011). "Aesthetic surgery of the female genitalia". Seminars in Plastic Surgery. 25 (2): 130–41. doi:10.1055/s-0031-1281482. PMC 3312147 . PMID 22547970.
- ↑ Braun, Virginia; Kitzinger, Celia (January 2001). "The perfectible vagina: Size matters". Culture, Health & Sexuality. 3 (3): 263–277. CiteSeerX 10.1.1.552.8931 . doi:10.1080/13691050152484704. S2CID 143982758.
- 1 2 Ritschel, Chelsea (29 January 2018). "The 'Husband Stitch' During Episiotomy Repair is a Disturbing Reality for Many New Mothers". The Independent. Archived from the original on 7 February 2018. Retrieved 9 February 2018.
- ↑ Transactions of the Texas State Medical Association. Vol. Seventeenth Annual Session. Houston, Texas: Texas State Medical Association. 21–23 April 1885.
- ↑ Imerman, Harold M.; Dewey, Thomas Blanchard (1958). What Women Want to Know: A Noted Gynecologist's Guide to the Personal Problems of Women's Health. New York: Crown. p. 134.
- ↑ Kitzinger, Sheila (1994). The Year After Childbirth: Surviving and Enjoying the First Year of Motherhood. HarperCollins Canada. ISBN 9780002550727.
- ↑ "Le point du mari, un vrai scandale?" [The husband stitch, a real scandal?]. elle.fr (in French). 2014-06-24. Retrieved 2023-03-10.
- 1 2 Jeantet, Diane (2014-04-18). "Derrière le " point du mari ", le traumatisme de l'épisiotomie" [Behind the “husband stitch”, the trauma of episiotomy]. Le Monde.fr (in French). Retrieved 2023-03-10.
- ↑ Hartmann, Katherine; Viswanathan, Meera; Palmieri, Rachel; Gartlehner, Gerald; Thorp, John; Lohr, Kathleen N. (2005-05-04). "Outcomes of Routine EpisiotomyA Systematic Review". JAMA. 293 (17): 2141–2148. doi:10.1001/jama.293.17.2141. ISSN 0098-7484. PMID 15870418.
- ↑ Jiang, Hong; Qian, Xu; Carroli, Guillermo; Garner, Paul (2017). "Selective versus routine use of episiotomy for vaginal birth". Cochrane Database of Systematic Reviews. 2017 (2): CD000081. doi:10.1002/14651858.CD000081.pub3. PMC 5449575 . PMID 28176333 . Retrieved 2023-03-10.
- ↑ Halton, Mary (26 April 2018). "The 'Husband Stitch' Leaves Women in Pain and Without Answers". Vice.
- ↑ Reilly, Kaitlin (21 February 2023). "Is 'the husband stitch' a medical myth? Women speak out about their experience". Yahoo Life. Retrieved 2023-03-10.
- ↑ Alam, Anam (2023-01-17). "Understanding the pain behind the 'husband stitch'". Thred Website. Retrieved 2023-03-10.
- ↑ Mezaguer, Louhann; auteurs-louhann_mezaguer (2021-11-26). "Point du mari : tout savoir sur cette mutilation gynécologique faite à l'insu des femmes en post-partum pour favoriser le plaisir de l'homme" [Husband stitch: everything you need to know about this gynecological mutilation carried out without the knowledge of postpartum women to promote the man's pleasure]. Grazia (in French). Retrieved 2023-03-10.
- ↑ Dobbeleir, Julie M. L. C. L.; Landuyt, Koenraad Van; Monstrey, Stan J. (May 2011). "Aesthetic Surgery of the Female Genitalia". Seminars in Plastic Surgery. 25 (2): 130–141. doi:10.1055/s-0031-1281482. ISSN 1535-2188. PMC 3312147 . PMID 22547970.
- ↑ Diniz, Simone G; Chacham, Alessandra S (2004-01-01). ""The Cut Above" and "the Cut Below": The Abuse of Caesareans and Episiotomy in São Paulo, Brazil". Reproductive Health Matters. 12 (23): 100–110. doi: 10.1016/S0968-8080(04)23112-3 . ISSN 0968-8080. PMID 15242215. S2CID 25469154.
- ↑ Schantz, Clémence; Sim, Kruy Leang; Ly, Ek Meng; Barennes, Hubert; Sudaroth, So; Goyet, Sophie (May 2015). "Reasons for routine episiotomy: A mixed-methods study in a large maternity hospital in Phnom Penh, Cambodia". Reproductive Health Matters. 23 (45): 68–77. doi: 10.1016/j.rhm.2015.06.012 . ISSN 1460-9576. PMID 26278834. S2CID 23339273.
- ↑ Machado, Carmen Maria (28 October 2014). "The Husband Stitch". Granta . Archived from the original on 28 January 2018. Retrieved 2 February 2018.
- ↑ "Make it Tighter: The Husband's Stitch". livewire.thewire.in. 2022-04-13. Retrieved 2023-01-30.
- ↑ "Colin From Accounts Season 1 Episode 4 Recap". reelmockery.com. 2022-04-13. Retrieved 2022-12-15.