An anxiolytic is a medication or other intervention that reduces anxiety. This effect is in contrast to anxiogenic agents which increase anxiety. Anxiolytic medications are used for the treatment of anxiety disorders and their related psychological and physical symptoms.
A dopamine reuptake inhibitor (DRI) is a class of drug which acts as a reuptake inhibitor of the monoamine neurotransmitter dopamine by blocking the action of the dopamine transporter (DAT). Reuptake inhibition is achieved when extracellular dopamine not absorbed by the postsynaptic neuron is blocked from re-entering the presynaptic neuron. This results in increased extracellular concentrations of dopamine and increase in dopaminergic neurotransmission.

Amantadine, sold under the brand name Gocovri among others, is a medication used to treat dyskinesia associated with parkinsonism and influenza caused by type A influenzavirus, though its use for the latter is no longer recommended because of widespread drug resistance. It acts as a nicotinic antagonist, dopamine agonist, and noncompetitive NMDA antagonist. The antiviral mechanism of action is antagonism of the influenzavirus A M2 proton channel, which prevents endosomal escape.

Phenylpiracetam, is a phenylated analog of the drug piracetam. It was developed in 1983 as a medication for Soviet Cosmonauts to treat the prolonged stresses of working in space. Phenylpiracetam was created at the Russian Academy of Sciences Institute of Biomedical Problems in an effort led by psychopharmacologist Valentina Ivanovna Akhapkina. In Russia it is now available as a prescription drug. Research on animals has indicated that phenylpiracetam may have anti-amnesic, antidepressant, anticonvulsant, anxiolytic, and memory enhancement effects.

Dopaminergic means "related to dopamine" (literally, "working on dopamine"), dopamine being a common neurotransmitter. Dopaminergic substances or actions increase dopamine-related activity in the brain. Dopaminergic brain pathways facilitate dopamine-related activity. For example, certain proteins such as the dopamine transporter (DAT), vesicular monoamine transporter 2 (VMAT2), and dopamine receptors can be classified as dopaminergic, and neurons that synthesize or contain dopamine and synapses with dopamine receptors in them may also be labeled as dopaminergic. Enzymes that regulate the biosynthesis or metabolism of dopamine such as aromatic L-amino acid decarboxylase or DOPA decarboxylase, monoamine oxidase (MAO), and catechol O-methyl transferase (COMT) may be referred to as dopaminergic as well. Also, any endogenous or exogenous chemical substance that acts to affect dopamine receptors or dopamine release through indirect actions (for example, on neurons that synapse onto neurons that release dopamine or express dopamine receptors) can also be said to have dopaminergic effects, two prominent examples being opioids, which enhance dopamine release indirectly in the reward pathways, and some substituted amphetamines, which enhance dopamine release directly by binding to and inhibiting VMAT2.

Punding is compulsive performance of repetitive, mechanical tasks, such as assembling and disassembling, collecting, or sorting objects. It can also apply to digital objects, such as computer files and data. The term was originally coined to describe complex, prolonged, purposeless, and stereotyped behaviour in phenmetrazine and chronic amphetamine users, by Swedish forensic psychiatrist G. Rylander, in 1968. It was later described in Parkinson's disease, but mainly in cases of patients being treated with dopaminergic drugs. It has also been described in methamphetamine and cocaine users, as well as in some patients with gambling addictions, and hypersexuality.
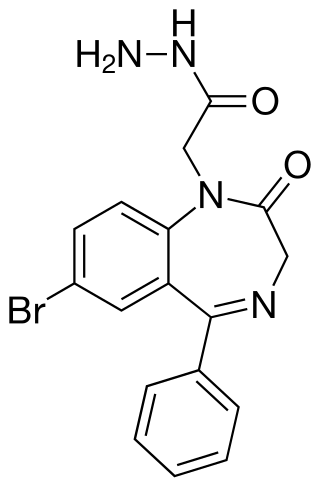
Gidazepam, also known as hydazepam or hidazepam, is a drug which is an atypical benzodiazepine derivative, developed in the Soviet Union. It is a selectively anxiolytic benzodiazepine. It also has therapeutic value in the management of certain cardiovascular disorders.
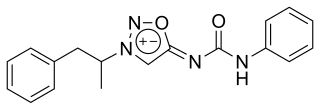
Mesocarb is a drug that is currently being developed for Parkinson's disease.

Latrepirdine is an antihistamine drug which has been used clinically in Russia since 1983.
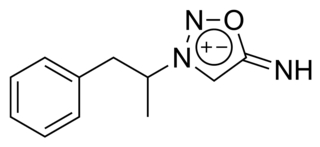
Feprosidnine (Sydnophen) is a stimulant drug which was developed in the USSR in the 1970s. It is structurally related to another Russian drug mesocarb but unlike mesocarb, was withdrawn earlier from production. In comparison with mesocarb it has own antidepressant activity, which makes it useful in treating depressions. Indications of feprosidnine included apathic, asthenic depressions, fatigue, apathic syndrome, narcolepsy and other similar conditions. Therapeutic range of doses: 10-50mg a day. Sydnophen has multiple mechanisms of action, the relative importance of which has not been clearly established. Effects on the body include reversible monoamine oxidase inhibition, cholinergic, adrenergic, opioid and nitric oxide donating actions, all of which may contribute to its pharmacological effects to some extent.

N-Phenylacetyl-l-prolylglycine ethyl ester is promoted as a nootropic and is a prodrug of cyclic glycine-proline. Other names include the brand name Noopept, developmental code GVS-111, and proposed INN omberacetam.

Fabomotizole is an anxiolytic drug launched in Russia in the early 2000s. It produces anxiolytic and neuroprotective effects without any sedative or muscle relaxant actions. Its mechanism of action remains poorly defined however, with GABAergic, NGF- and BDNF-release-promoting, MT1 receptor agonism, MT3 receptor antagonism, and sigma agonism suggested as potential mechanisms. Fabomotizole was shown to inhibit MAO-A reversibly and there might be also some involvement with serotonin receptors. Clinical trials have shown fabomotizole to be well tolerated and reasonably effective for the treatment of anxiety.

Selank is a nootropic, anxiolytic peptide based drug developed by the Institute of Molecular Genetics of the Russian Academy of Sciences. Selank is a heptapeptide with the sequence Thr-Lys-Pro-Arg-Pro-Gly-Pro (TKPRPGP). It is a synthetic analogue of human tuftsin.

Emoxypine (2-ethyl-6-methyl-3-hydroxypyridine), also known as Mexidol or Mexifin, a succinate salt, is chemical compound which is claimed by its manufacturer, the Russian company Pharmasoft Pharmaceuticals, to have antioxidant and actoprotector properties.

Nooglutyl is a nootropic agent that was studied at the Research Institute of Pharmacology, Russian Academy of Medical Sciences as a potential treatment for amnesia.
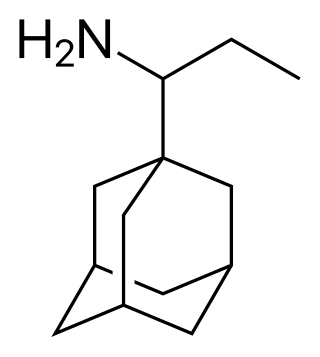
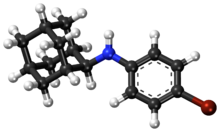
Adapromine is an antiviral drug of the adamantane group related to amantadine (1-aminoadamantane), rimantadine, and memantine (1-amino-3,5-dimethyladamantane) that is marketed in Russia for the treatment and prevention of influenza. It is an alkyl analogue of rimantadine and is similar to rimantadine in its antiviral activity but possesses a broader spectrum of action, being effective against influenza viruses of both type A and B. Strains of type A influenza virus with resistance to adapromine and rimantadine and the related drug deitiforine were encountered in Mongolia and the Soviet Union in the 1980s.

Arabinopyranosyl-N-methyl-N-nitrosourea, also known as Aranose (Араноза) is a cytostatic anticancer chemotherapeutic drug of an alkylating type. Chemically it is a nitrosourea derivative. It was developed in the Soviet Union in the 1970s. It was claimed by its developers that its advantages over other nitrosoureas are a relatively low hematological toxicity and a wider therapeutic index, which allows for its outpatient administration.

Tolibut, also known as 3-(p-tolyl)-4-aminobutyric acid (or β-(4-methylphenyl)-GABA), is drug that was developed in Russia. It is an analogue of γ-aminobutyric acid (GABA) and is the 4-methyl analogue of phenibut, and is also an analogue of baclofen where the 4-chloro substitution has been replaced with a 4-methyl substitution. Tolibut has been described as possessing analgesic, tranquilizing, and neuroprotective properties. It is not fully clear as to whether the drug was ever approved or used medically in Russia.
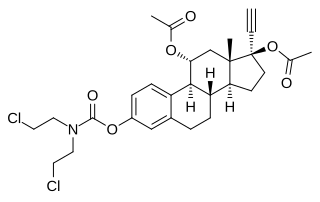
Cytestrol acetate is a steroidal antiestrogen and a cytostatic antineoplastic agent which was developed for the treatment of breast cancer but was never marketed.
Actoprotectors or synthetic adaptogens are compounds that enhance an organism's resilience to physical stress without increasing heat output. Actoprotectors are distinct from other performance-enhancing substances in that they increase physical and psychological resilience via non-exhaustive action. The term "actoprotector" is used to describe synthetic and isolated compounds possessing adaptogenic properties. By contrast, the term "adaptogen" is most often use to describe a natural herb as a whole, which can contain hundreds if not thousands of biologically active components.