
Ectopic pregnancy is a complication of pregnancy in which the embryo attaches outside the uterus. Signs and symptoms classically include abdominal pain and vaginal bleeding, but fewer than 50 percent of affected women have both of these symptoms. The pain may be described as sharp, dull, or crampy. Pain may also spread to the shoulder if bleeding into the abdomen has occurred. Severe bleeding may result in a fast heart rate, fainting, or shock. With very rare exceptions, the fetus is unable to survive.
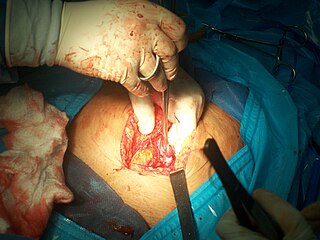
Tubal ligation is a surgical procedure for female sterilization in which the fallopian tubes are permanently blocked, clipped or removed. This prevents the fertilization of eggs by sperm and thus the implantation of a fertilized egg. Tubal ligation is considered a permanent method of sterilization and birth control.
Gamete intrafallopian transfer (GIFT) is a tool of assisted reproductive technology against infertility. Eggs are removed from a woman's ovaries, and placed in one of the fallopian tubes, along with the man's sperm. The technique, first attempted by Steptoe and Edwards and later pioneered by endocrinologist Ricardo Asch, allows fertilization to take place inside the woman's uterus.

Asherman's syndrome (AS) is an acquired uterine condition that occurs when scar tissue (adhesions) forms inside the uterus and/or the cervix. It is characterized by variable scarring inside the uterine cavity, where in many cases the front and back walls of the uterus stick to one another. AS can be the cause of menstrual disturbances, infertility, and placental abnormalities. Although the first case of intrauterine adhesion was published in 1894 by Heinrich Fritsch, it was only after 54 years that a full description of Asherman syndrome was carried out by Joseph Asherman. A number of other terms have been used to describe the condition and related conditions including: uterine/cervical atresia, traumatic uterine atrophy, sclerotic endometrium, and endometrial sclerosis.
Zygote intra fallopian transfer (ZIFT) is an infertility treatment used when a blockage in the fallopian tubes prevents the normal binding of sperm to the egg. Egg cells are removed from a woman's ovaries, and in vitro fertilised. The resulting zygote is placed into the fallopian tube by the use of laparoscopy. The procedure is a spin-off of the gamete intrafallopian transfer (GIFT) procedure. The pregnancy and implantation rates in ZIFT cycles are 52.3 and 23.2% which were higher than what was observed in IVF cycles which were 17.5 and 9.7%.

Hysteroscopy is the inspection of the uterine cavity by endoscopy with access through the cervix. It allows for the diagnosis of intrauterine pathology and serves as a method for surgical intervention.
Tuboplasty refers to a number of surgical operations that attempt to restore patency and functioning of the fallopian tube(s) so that a pregnancy could be achieved. As tubal infertility is a common cause of infertility, tuboplasties were commonly performed prior to the development of effective in vitro fertilization (IVF) or repair of any type of tube-like structure, including the Eustachian tube in the head and neck.

Essure was a device for female sterilization. It is a metal coil which when placed into each fallopian tube induces fibrosis and blockage. Essure was designed as an alternative to tubal ligation. However, it was recalled by Bayer in 2018, and the device is no longer sold due to complications secondary to its implantation. The company has reported that several patients implanted with the Essure System for Permanent Birth Control have experienced and/or reported adverse effects, including: perforation of the uterus and/or fallopian tubes, identification of inserts in the abdominal or pelvic cavity, persistent pain, and suspected allergic or hypersensitivity reaction. Although designed to remain in place for a lifetime, it was approved based on short-term safety studies. Of the 745 women with implants in the original premarket studies, 92% were followed up at one year, and 25% for two years, for safety outcomes. A 2009 review concluded that Essure appeared safe and effective based on short-term studies, that it was less invasive and could be cheaper than laparoscopic bilateral tubal ligation. About 750,000 women have received the device worldwide.

A hydrosalpinx is a condition that occurs when a fallopian tube is blocked and fills with serous or clear fluid near the ovary. The blocked tube may become substantially distended giving the tube a characteristic sausage-like or retort-like shape. The condition is often bilateral and the affected tubes may reach several centimeters in diameter. The blocked tubes cause infertility. A fallopian tube filled with blood is a hematosalpinx, and with pus a pyosalpinx.
Tubal reversal, also called tubal sterilization reversal, tubal ligation reversal, or microsurgical tubal reanastomosis, is a surgical procedure that can restore fertility to women after a tubal ligation. By rejoining the separated segments of the fallopian tube, tubal reversal can give women the chance to become pregnant again. In some cases, however, the separated segments cannot actually be reattached to each other. In some cases the remaining segment of tube needs to be re-implanted into the uterus. In other cases, when the end of the tube has been removed, a procedure called a neofimbrioplasty must be performed to recreate a functional end of the tube which can then act like the missing fimbria and retrieve the egg that has been released during ovulation.

Fallopian tube obstruction, also known as fallopian tube occlusion is a major cause of female infertility. Blocked fallopian tubes are unable to let the ovum and the sperm converge, thus making fertilization impossible. Fallopian tubes are also known as oviducts, uterine tubes, and salpinges.
The fertiloscope is a type of laparoscope, modified to make it suitable for trans-vaginal application, which is used in the diagnosis and treatment of female infertility.

The fallopian tubes, also known as uterine tubes, oviducts or salpinges, are paired tubes in the human female body that stretch from the uterus to the ovaries. The fallopian tubes are part of the female reproductive system. In other mammals they are only called oviducts.

Salpingitis isthmica nodosa (SIN), also known as diverticulosis of the Fallopian tube, is nodular thickening of the narrow part of the uterine tube, due to inflammation.

Fertility testing is the process by which fertility is assessed, both generally and also to find the "fertile window" in the menstrual cycle. General health affects fertility, and STI testing is an important related field.

Hysterosalpingography (HSG), also known as uterosalpingography, is a radiologic procedure to investigate the shape of the uterine cavity and the shape and patency of the Fallopian tubes. It is a special x-ray procedure using dye to look at the womb (uterus) and Fallopian tubes. In this procedure a radio-opaque material is injected into the cervical canal, and radiographs are taken. A normal result shows the filling of the uterine cavity and the bilateral filling of the Fallopian tube with the injection material. To demonstrate tubal rupture, spillage of the material into the peritoneal cavity needs to be observed. Hysterosalpingography has vital role in treatment of infertility, especially in the case of fallopian tube blockage.
Sonosalpingography (SSG), also known as Sion test, is a diagnostic procedure primarily used for evaluating patency of fallopian tubes. It was introduced as a screening procedure for infertility investigations. It is becoming more popular among practitioners due to absence of side effects.
Endometriosis and its complications are a major cause of female infertility. Endometriosis is a dysfunction characterized by the migration of endometrial tissue to areas outside of the endometrium of the uterus. The most common places to find stray tissue are on ovaries and fallopian tubes, followed by other organs in the lower abdominal cavity such as the bladder and intestines. Typically, the endometrial tissue adheres to the exteriors of the organs, and then creates attachments of scar tissue called adhesions that can join adjacent organs together. The endometrial tissue and the adhesions can block a fallopian tube and prevent the meeting of ovum and sperm cells, or otherwise interfere with fertilization, implantation and, rarely, the carrying of the fetus to term.

Tubal factor infertility (TFI) is female infertility caused by diseases, obstructions, damage, scarring, congenital malformations or other factors which impede the descent of a fertilized or unfertilized ovum into the uterus through the Fallopian tubes and prevents a normal pregnancy and full term birth. Tubal factors cause 25-30% of infertility cases. Tubal factor is one complication of Chlamydia trachomatis infection in women.
Chromopertubation is a method for the study of fallopian tube patency for suspected infertility in women caused by fallopian tube obstruction. Occlusion or pathology of the fallopian tubes is the most common cause of suspected infertility. Chromopertubation is sometimes commonly referred to a "laparoscopy and dye" test. It is currently one of the standard procedures in this field. In most cases, chromopertubation is performed to assess and determine the cause of someone's difficulties in getting pregnant.











