
Prenatal care, also known as antenatal care, is a type of preventive healthcare. It is provided in the form of medical checkups, consisting of recommendations on managing a healthy lifestyle and the provision of medical information such as maternal physiological changes in pregnancy, biological changes, and prenatal nutrition including prenatal vitamins, which prevents potential health problems throughout the course of the pregnancy and promotes the mother and child's health alike.The availability of routine prenatal care, including prenatal screening and diagnosis, has played a part in reducing the frequency of maternal death, miscarriages, birth defects, low birth weight, neonatal infections and other preventable health problems.

Obstetric ultrasonography, or prenatal ultrasound, is the use of medical ultrasonography in pregnancy, in which sound waves are used to create real-time visual images of the developing embryo or fetus in the uterus (womb). The procedure is a standard part of prenatal care in many countries, as it can provide a variety of information about the health of the mother, the timing and progress of the pregnancy, and the health and development of the embryo or fetus.
Oligohydramnios is a medical condition in pregnancy characterized by a deficiency of amniotic fluid, the fluid that surrounds the fetus in the abdomen, in the amniotic sac. It is typically diagnosed by ultrasound when the amniotic fluid index (AFI) measures less than 5 cm or when the single deepest pocket (SDP) of amniotic fluid measures less than 2 cm. Amniotic fluid is necessary to allow for normal fetal movement, lung development, and cushioning from uterine compression. Low amniotic fluid can be attributed to a maternal, fetal, placental or idiopathic cause and can result in poor fetal outcomes including death. The prognosis of the fetus is dependent on the etiology, gestational age at diagnosis, and the severity of the oligohydramnios.

Small for gestational age (SGA) newborns are those who are smaller in size than normal for the gestational age, most commonly defined as a weight below the 10th percentile for the gestational age.
The triple test, also called triple screen, the Kettering test or the Bart's test, is an investigation performed during pregnancy in the second trimester to classify a patient as either high-risk or low-risk for chromosomal abnormalities.
In obstetrics, gestational age is a measure of the age of a pregnancy which is taken from the beginning of the woman's last menstrual period (LMP), or the corresponding age of the gestation as estimated by a more accurate method if available. Such methods include adding 14 days to a known duration since fertilization, or by obstetric ultrasonography. The popularity of using this definition of gestational age is that menstrual periods are essentially always noticed, while there is usually a lack of a convenient way to discern when fertilization occurred. "Gestational age" in other contexts may mean embryonic age.

Pregnancy is the time during which one or more offspring develops (gestates) inside a woman's womb. A multiple pregnancy involves more than one offspring, such as with twins. Pregnancy usually occurs by sexual intercourse, but can also occur through assisted reproductive technology procedures. A pregnancy may end in a live birth, a spontaneous miscarriage, an induced abortion, or a stillbirth. Childbirth typically occurs around 40 weeks from the start of the last menstrual period (LMP), a span known as the gestational age. This is just over nine months. Counting by fertilization age, the length is about 38 weeks. Pregnancy is "the presence of an implanted human embryo or fetus in the uterus"; implantation occurs on average 8–9 days after fertilization. An embryo is the term for the developing offspring during the first seven weeks following implantation, after which the term fetus is used until birth. Signs and symptoms of early pregnancy may include missed periods, tender breasts, morning sickness, hunger, and frequent urination. Pregnancy may be confirmed with a pregnancy test. Methods of birth control—or, more accurately, contraception—are used to avoid pregnancy.

Large for gestational age (LGA) is a term used to describe infants that are born with an abnormally high weight, specifically in the 90th percentile or above, compared to other babies of the same developmental age. Macrosomia is a similar term that describes excessive birth weight, but refers to an absolute measurement, regardless of gestational age. Typically the threshold for diagnosing macrosomia is a body weight of between 4,000 and 4,500 grams, or more, measured at birth, but there are difficulties reaching a universal agreement of this definition.
Prenatal development includes the development of the embryo and of the foetus during a viviparous animal's gestation. Prenatal development starts with fertilization, in the germinal stage of embryonic development, and continues in fetal development until birth.

Fetal surgery also known as antenatal surgery, prenatal surgery, is a growing branch of maternal-fetal medicine that covers any of a broad range of surgical techniques that are used to treat birth defects in fetuses who are still in the pregnant uterus. There are three main types: open fetal surgery, which involves completely opening the uterus to operate on the fetus; minimally invasive fetoscopic surgery, which uses small incisions and is guided by fetoscopy and sonography; and percutaneous fetal therapy, which involves placing a catheter under continuous ultrasound guidance.
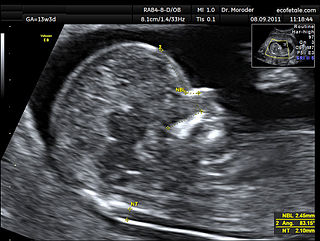
A nuchal scan or nuchal translucency (NT) scan/procedure is a sonographic prenatal screening scan (ultrasound) to detect chromosomal abnormalities in a fetus, though altered extracellular matrix composition and limited lymphatic drainage can also be detected.

A bicornuate uterus or bicornate uterus, is a type of mullerian anomaly in the human uterus, where there is a deep indentation at the fundus (top) of the uterus.
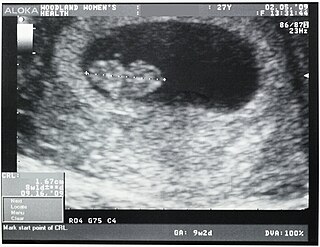
Crown-rump length (CRL) is the measurement of the length of human embryos and fetuses from the top of the head (crown) to the bottom of the buttocks (rump). It is typically determined from ultrasound imagery and can be used to estimate gestational age.

Cephalometry is the study and measurement of the head, usually the human head, especially by medical imaging such as radiography. Craniometry, the measurement of the cranium (skull), is a large subset of cephalometry. Cephalometry also has a history in phrenology, which is the study of personality and character as well as physiognomy, which is the study of facial features. Cephalometry as applied in a comparative anatomy context informs biological anthropology. In clinical contexts such as dentistry and oral and maxillofacial surgery, cephalometric analysis helps in treatment and research; cephalometric landmarks guide surgeons in planning and operating.
The estimated date of delivery (EDD), also known as expected date of confinement, and estimated due date or simply due date, is a term describing the estimated delivery date for a pregnant woman. Normal pregnancies last between 38 and 42 weeks. Children are delivered on their expected due date about 4% of the time.
Post-maturity syndrome develops in about 20% of human pregnancies continuing past the expected dates. Ten years ago it was generally held that the postmature fetus ran some risk of dying in the uterus before the onset of labour because of degeneration and calcification of the placenta. Features of post-maturity syndrome include oligohydramnios, meconium aspiration, macrosomia and fetal problems such as dry peeling skin, overgrown nails, abundant scalp hair, visible creases on palms and soles, minimal fat deposition and skin colour become green or yellow due to meconeum staining. Post-maturity refers to any baby born after 42 weeks gestation or 294 days past the first day of the mother's last menstrual period. Less than 6 percent of all babies are born at 42 weeks or later. In most cases, continued fetal growth between 39 and 43 wk gestation results in a macrosomic infant. However, sometimes the placenta involutes, and multiple infarcts and villous degeneration cause placental insufficiency syndrome. In this syndrome, the fetus receives inadequate nutrients and oxygen from the mother, resulting in a thin, small-for-gestational-age, undernourished infant with depleted glycogen stores. Post term, the amniotic fluid volume eventually decreases, leading to oligohydramnios. Although pregnancy is said to last nine months, health care providers track pregnancy by weeks and days. The estimated delivery date, also called the estimated due date or EDD, is calculated as 40 weeks or 280 days from the first day of the last menstrual period. Only 4 percent women will deliver on their due date. The terms Post-maturity or "Post-term" are both words used to describe babies born after 42 weeks. The terms "post-maturity" and "post-term" are interchangeable. As there are many definitions for prolonged pregnancy the incidence varies from 2 to 10%.When incidence is taken as delivery beyond 42 weeks it is 10%, if it is taken according to the delivered baby's weight and length it is 2%.The baby may have birth weight of 4kg and length of 54 cm but these findings are variable, even the baby may have underweight. Post-maturity is more likely to happen when a mother has had a post-term pregnancy before. After one post-term pregnancy, the risk of a second post-term birth increases by 2 to 3 times. Other, minor risk factors include an older or obese mother, a white mother, male baby, or a family history of post-maturity. Maternal risks include obstructed labor, perennial damage, instrumental vaginal delivery, a Cesarean section, infection, and post postpartum hemorrhage. Accurate pregnancy due dates can help identify babies at risk for post-maturity. Ultrasound examinations early in pregnancy help establish more accurate dating by measurements taken of the fetus. Pregnancies complicated by gestational diabetes, hypertension, or other high-risk conditions should be managed according to guidelines for those conditions.

Prenatal nutrition addresses nutrient recommendations before and during pregnancy. Nutrition and weight management before and during pregnancy has a profound effect on the development of infants. This is a rather critical time for healthy development since infants rely heavily on maternal stores and nutrient for optimal growth and health outcome later in life.
Anthropometry is defined as the scientific study of the human body measurements and proportions. These studies are generally used by clinicians and pathologists for adequate assessments of the growth and development of the fetus at any specific point of gestational maturity. Fetal height, fetal weight, head circumference (HC), crown to rump length (CR), dermatological observations like skin thickness etc. are measured individually to assess the growth and development of the organs and the fetus as a whole and can be a parameter for normal or abnormal development also including adaptation of the fetus to its newer environment.
The anomaly scan, also sometimes called the anatomy scan, 20-week ultrasound, or level 2 ultrasound, evaluates anatomic structures of the fetus, placenta, and maternal pelvic organs. This scan is an important and common component of routine prenatal care. The function of the ultrasound is to measure the fetus so that growth abnormalities can be recognized quickly later in pregnancy, and to assess for congenital malformations and multiple pregnancies.

The Pregnancy Outcome Prediction (POP) Study is a prospective cohort study of 4,512 women that have never given birth recruited at the Rosie Hospital between January 2008 and July 2012.












