Related Research Articles

An abscess is a collection of pus that has built up within the tissue of the body. Signs and symptoms of abscesses include redness, pain, warmth, and swelling. The swelling may feel fluid-filled when pressed. The area of redness often extends beyond the swelling. Carbuncles and boils are types of abscess that often involve hair follicles, with carbuncles being larger. A cyst is related to an abscess, but it contains a material other than pus, and a cyst has a clearly defined wall.

Necrosis is a form of cell injury which results in the premature death of cells in living tissue by autolysis. The term "necrosis" came about in the mid-19th century and is commonly attributed to German pathologist Rudolf Virchow, who is often regarded as one of the founders of modern pathology. Necrosis is caused by factors external to the cell or tissue, such as infection, or trauma which result in the unregulated digestion of cell components. In contrast, apoptosis is a naturally occurring programmed and targeted cause of cellular death. While apoptosis often provides beneficial effects to the organism, necrosis is almost always detrimental and can be fatal.

Sputum is mucus that is coughed up from the lower airways. In medicine, sputum samples are usually used for a naked eye examination, microbiological investigation of respiratory infections and cytological investigations of respiratory systems. It is crucial that the specimen does not include any mucoid material from the nose or oral cavity.

Entamoeba histolytica is an anaerobic parasitic amoebozoan, part of the genus Entamoeba. Predominantly infecting humans and other primates causing amoebiasis, E. histolytica is estimated to infect about 35-50 million people worldwide. E. histolytica infection is estimated to kill more than 55,000 people each year. Previously, it was thought that 10% of the world population was infected, but these figures predate the recognition that at least 90% of these infections were due to a second species, E. dispar. Mammals such as dogs and cats can become infected transiently, but are not thought to contribute significantly to transmission.
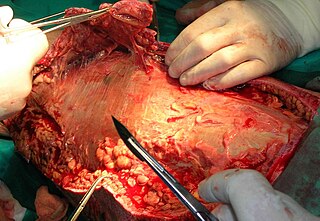
Debridement is the medical removal of dead, damaged, or infected tissue to improve the healing potential of the remaining healthy tissue. Removal may be surgical, mechanical, chemical, autolytic (self-digestion), and by maggot therapy.

Dystrophic calcification (DC) is the calcification occurring in degenerated or necrotic tissue, as in hyalinized scars, degenerated foci in leiomyomas, and caseous nodules. This occurs as a reaction to tissue damage, including as a consequence of medical device implantation. Dystrophic calcification can occur even if the amount of calcium in the blood is not elevated, in contrast to metastatic calcification, which is a consequence of a systemic mineral imbalance, including hypercalcemia and/or hyperphosphatemia, that leads to calcium deposition in healthy tissues. In dystrophic calcification, basophilic calcium salt deposits aggregate, first in the mitochondria, then progressively throughout the cell. These calcifications are an indication of previous microscopic cell injury, occurring in areas of cell necrosis when activated phosphatases bind calcium ions to phospholipids in the membrane.

Toothache, also known as dental pain or tooth pain, is pain in the teeth or their supporting structures, caused by dental diseases or pain referred to the teeth by non-dental diseases. When severe it may impact sleep, eating, and other daily activities.
Coagulative necrosis is a type of accidental cell death typically caused by ischemia or infarction. In coagulative necrosis, the architectures of dead tissue are preserved for at least a couple of days. It is believed that the injury denatures structural proteins as well as lysosomal enzymes, thus blocking the proteolysis of the damaged cells. The lack of lysosomal enzymes allows it to maintain a "coagulated" morphology for some time. Like most types of necrosis, if enough viable cells are present around the affected area, regeneration will usually occur. Coagulative necrosis occurs in most bodily organs, excluding the brain. Different diseases are associated with coagulative necrosis, including acute tubular necrosis and acute myocardial infarction.

Lung abscess is a type of liquefactive necrosis of the lung tissue and formation of cavities containing necrotic debris or fluid caused by microbial infection.

Gas gangrene is a bacterial infection that produces tissue gas in gangrene. This deadly form of gangrene usually is caused by Clostridium perfringens bacteria. About 1,000 cases of gas gangrene are reported yearly in the United States.

Pericoronitis is inflammation of the soft tissues surrounding the crown of a partially erupted tooth, including the gingiva (gums) and the dental follicle. The soft tissue covering a partially erupted tooth is known as an operculum, an area which can be difficult to access with normal oral hygiene methods. The hyponym operculitis technically refers to inflammation of the operculum alone.
A phlegmon is a localized area of acute inflammation of the soft tissues. It is a descriptive term which may be used for inflammation related to a bacterial infection or non-infectious causes. Most commonly, it is used in contradistinction to a "walled-off" pus-filled collection (abscess), although a phlegmon may progress to an abscess if untreated. A phlegmon can localize anywhere in the body. The Latin term phlegmōn is from Ancient Greek φλέγω (phlégō) 'burn'.
Pancreatic diseases are diseases that affect the pancreas, an organ in most vertebrates and in humans and other mammals located in the abdomen. The pancreas plays a role in the digestive and endocrine system, producing enzymes which aid the digestion process and the hormone insulin, which regulates blood sugar levels. The most common pancreatic disease is pancreatitis, an inflammation of the pancreas which could come in acute or chronic form. Other pancreatic diseases include diabetes mellitus, exocrine pancreatic insufficiency, cystic fibrosis, pseudocysts, cysts, congenital malformations, tumors including pancreatic cancer, and hemosuccus pancreaticus.

Sialadenitis (sialoadenitis) is inflammation of salivary glands, usually the major ones, the most common being the parotid gland, followed by submandibular and sublingual glands. It should not be confused with sialadenosis (sialosis) which is a non-inflammatory enlargement of the major salivary glands.
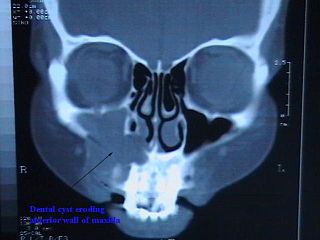
Commonly known as a dental cyst, the periapical cyst is the most common odontogenic cyst. It may develop rapidly from a periapical granuloma, as a consequence of untreated chronic periapical periodontitis.

Amoebic brain abscess is an affliction caused by the anaerobic parasitic protist Entamoeba histolytica. It is extremely rare; the first case being reported in 1849. Brain abscesses resulting from Entamoeba histolytica are difficult to diagnose and very few case reports suggest complete recovery even after the administration of appropriate treatment regimen.
Pulp necrosis is a clinical diagnostic category indicating the death of cells and tissues in the pulp chamber of a tooth with or without bacterial invasion. It is often the result of many cases of dental trauma, caries and irreversible pulpitis.
Citrobacter koseri, formerly known as Citrobacter diversus, is a Gram-negative non-spore forming, rod-shaped bacterium. It is a facultative anaerobe capable of aerobic respiration. It is motile via peritrichous flagella. It is a member of the family of Enterobacteriaceae. The members of this family are part of the normal flora and commonly found in the digestive tracts of humans and animals.C. koseri may act as an opportunistic pathogen in individuals who are immunocompromised.
Anaerobic infections are caused by anaerobic bacteria. Obligately anaerobic bacteria do not grow on solid media in room air ; facultatively anaerobic bacteria can grow in the presence or absence of air. Microaerophilic bacteria do not grow at all aerobically or grow poorly, but grow better under 10% carbon dioxide or anaerobically. Anaerobic bacteria can be divided into strict anaerobes that can not grow in the presence of more than 0.5% oxygen and moderate anaerobic bacteria that are able of growing between 2 and 8% oxygen. Anaerobic bacteria usually do not possess catalase, but some can generate superoxide dismutase which protects them from oxygen.

A lung cavity or pulmonary cavity is an abnormal, thick-walled, air-filled space within the lung. Cavities in the lung can be caused by infections, cancer, autoimmune conditions, trauma, congenital defects, or pulmonary embolism. The most common cause of a single lung cavity is lung cancer. Bacterial, mycobacterial, and fungal infections are common causes of lung cavities. Globally, tuberculosis is likely the most common infectious cause of lung cavities. Less commonly, parasitic infections can cause cavities. Viral infections almost never cause cavities. The terms cavity and cyst are frequently used interchangeably; however, a cavity is thick walled, while a cyst is thin walled. The distinction is important because cystic lesions are unlikely to be cancer, while cavitary lesions are often caused by cancer.
References
- 1 2 3 Robbins and Cotran: Pathologic Basis of Disease, 8th Ed. 2010. Pg. 15
- ↑ Ngan, Vanessa. "Chemical burn". DermNet New Zealand. Retrieved 4 February 2018.
- ↑ "Cell Injury" . Retrieved 2009-05-15.
- ↑ Quaia E, Baratella E, Pizzolato R, Bussani R, Cova MA (March 2009). "Radiological-pathological correlation in intratumoural tissue components of solid lung tumours". Radiol Med. 114 (2): 173–89. doi:10.1007/s11547-008-0354-6. PMID 19082781. S2CID 12867674.