Causes
| | This section is empty. You can help by adding to it. (April 2020) |
Penoscrotal transposition (PST) is a group of congenital defects involving an abnormal spatial arrangement of penis and scrotum.
There are two types of penoscrotal transposition. [1]
In incomplete penoscrotal transposition, penis is located in the middle of the scrotum, but in complete transposition, penis is located in the perineum. [2]
| | This section is empty. You can help by adding to it. (April 2020) |
Gold standard of PST treatment is surgical repair. [2] Repair technique of penoscrotal transposition included a Glenn–Anderson technique, which is developed by F. Glenn and E. Everett Anderson. [3] [4]

Foreskin restoration is the process of expanding the skin on the penis to reconstruct an organ similar to the foreskin, which has been removed by circumcision or injury. Foreskin restoration is primarily accomplished by stretching the residual skin of the penis, but surgical methods also exist. Restoration creates a facsimile of the foreskin, but specialized tissues removed during circumcision cannot be reclaimed. Actual regeneration of the foreskin is experimental at this time. Some forms of restoration involve only partial regeneration in instances of a high-cut wherein the circumcisee feels that the circumciser removed too much skin and that there is not enough skin for erections to be comfortable.

Hypospadias is a common variation in fetal development of the penis in which the urethra does not open from its usual location on the head of the penis. It is the second-most common birth defect of the male reproductive system, affecting about one of every 250 males at birth. Roughly 90% of cases are the less serious distal hypospadias, in which the urethral opening is on or near the head of the penis (glans). The remainder have proximal hypospadias, in which the meatus is all the way back on the shaft of the penis, near or within the scrotum. Shiny tissue that typically forms the urethra instead extends from the meatus to the tip of the glans; this tissue is called the urethral plate.
Phalloplasty is the construction or reconstruction of a penis or the artificial modification of the penis by surgery. The term is also occasionally used to refer to penis enlargement.

Orchiopexy is a surgery to move and/or permanently fix a testicle into the scrotum. While orchiopexy typically describes the operation to surgically correct an undescended testicle, it is also used to resolve testicular torsion.

Intersex medical interventions, also known as intersex genital mutilations (IGM), are surgical, hormonal and other medical interventions performed to modify atypical or ambiguous genitalia and other sex characteristics, primarily for the purposes of making a person's appearance more typical and to reduce the likelihood of future problems. The history of intersex surgery has been characterized by controversy due to reports that surgery can compromise sexual function and sensation, and create lifelong health issues. Timing, evidence, necessity and indications for surgeries in infancy, adolescence or adult age have been controversial, associated with issues of consent.
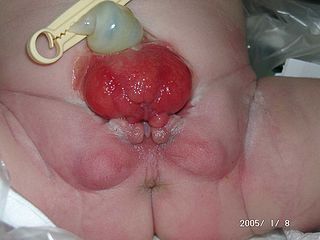
Bladder exstrophy is a congenital anomaly that exists along the spectrum of the exstrophy-epispadias complex, and most notably involves protrusion of the urinary bladder through a defect in the abdominal wall. Its presentation is variable, often including abnormalities of the bony pelvis, pelvic floor, and genitalia. The underlying embryologic mechanism leading to bladder exstrophy is unknown, though it is thought to be in part due to failed reinforcement of the cloacal membrane by underlying mesoderm. Exstrophy means the inversion of a hollow organ.

Scrotoplasty, also known as oscheoplasty, is a type of surgery to create or repair the scrotum. The history of male genital plastic surgery is rooted in many cultures and dates back to ancient times. However, scientific research for male genital plastic surgery such as scrotoplasty began to develop in the early 1900s. The development of testicular implants began in 1940 made from materials outside of what is used today. Today, testicular implants are created from saline or gel filled silicone rubber. There are a variety of reasons why scrotoplasty is done. Some transgender men and intersex or non-binary people who were assigned female at birth may choose to have this surgery to create a scrotum, as part of their transition. Other reasons for this procedure include addressing issues with the scrotum due to birth defects, aging, or medical conditions such as infection. For newborn males with penoscrotal defects such as webbed penis, a condition in which the penile shaft is attached to the scrotum, scrotoplasty can be performed to restore normal appearance and function. For older male adults, the scrotum may extend with age. Scrotoplasty or scrotal lift can be performed to remove the loose, excess skin. Scrotoplasty can also be performed for males who undergo infection, necrosis, traumatic injury of the scrotum.

The frenulum of the penis, often known simply as the frenulum or frenum, is a thin elastic strip of tissue on the underside of the glans and the neck of the human penis. In men who are not circumcised, it also connects the foreskin to the glans and the ventral mucosa. In adults, the frenulum is typically supple enough to allow manual movement of the foreskin over the glans and help retract the foreskin during erection. In flaccid state, it tightens to narrow the foreskin opening.

A penile implant is an implanted device intended for the treatment of erectile dysfunction, Peyronie's disease, ischemic priapism, deformity and any traumatic injury of the penis, and for phalloplasty or metoidioplasty, including in gender-affirming surgery. Men also opt for penile implants for aesthetic purposes. Men's satisfaction and sexual function is influenced by discomfort over genital size which leads to seek surgical and non-surgical solutions for penis alteration. Although there are many distinct types of implants, most fall into one of two categories: malleable and inflatable transplants.
Post-vasectomy pain syndrome (PVPS) is a chronic and sometimes debilitating genital pain condition that may develop immediately or several years after vasectomy. Because this condition is a syndrome, there is no single treatment method, therefore efforts focus on mitigating/relieving the individual patient's specific pain. When pain in the epididymides is the primary symptom, post-vasectomy pain syndrome is often described as congestive epididymitis.
Urethroplasty is the surgical repair of an injury or defect within the walls of the urethra. Trauma, iatrogenic injury and infections are the most common causes of urethral injury/defect requiring repair. Urethroplasty is regarded as the gold standard treatment for urethral strictures and offers better outcomes in terms of recurrence rates than dilatations and urethrotomies. It is probably the only useful modality of treatment for long and complex strictures though recurrence rates are higher for this difficult treatment group.

The corona of glans penis or penis crown refers to the rounded projecting border or flare that forms at the base of the glans in human males. The corona overhangs a mucosal surface, known as the neck of the penis, which separates the shaft and the glans. The deep retro-glandular coronal sulcus forms between the corona and the neck of the penis. The two sides of the corona merge on the ventral midline forming the septum glandis. The circumference of the corona is richly innervated and is described as a highly erogenous area of the glans.

Mani Menon, born 9 July 1948 in Trichur, India, is an American surgeon whose work has helped to lay the foundation for modern Robotic Cancer Surgery. He is the founding director and the Raj and Padma Vattikuti Distinguished Chair of the Vattikuti Urology Institute at the Henry Ford Hospital in Detroit, MI, where he established the first cancer-oriented robotics program in the world. Menon is widely regarded for his role in the development of robotic surgery techniques for the treatment of patients with prostate, kidney, and bladder cancers, as well as for the development of robotic kidney transplantation.
Menon is the recipient of the Gold Cystoscope award, Hugh Hampton Young award, the Keyes Medal, the prestigious B.C. Roy award.

Buried penis, also called hidden penis or retractile penis, is a congenital or acquired condition in which the penis is partially or completely hidden below the surface of the skin. A buried penis can lead to urinary difficulties, poor hygiene, infection, and inhibition of normal sexual function.
Ectopic testis is used to describe the testis leaving the inguinal canal and entering a site other than the scrotum. Usually, it results from obstruction of the scrotal entrance or from overdevelopment and lengthening of a segment of the gubernaculum.

Webbed penis also known as buried or concealed penis is an acquired or congenital condition in which the scrotal skin extends onto the ventral penile shaft. The penile shaft is buried in the scrotum or tethered to the scrotal midline by a fold or web of skin. The urethra and erectile bodies are usually normal. Webbed penis is usually asymptomatic, but the cosmetic appearance is often unacceptable. This condition may be corrected by surgical techniques.

An artificial urinary sphincter (AUS) is an implanted device to treat moderate to severe stress urinary incontinence, most commonly in men. The AUS is designed to supplement the function of the natural urinary sphincter that restricts urine flow out of the bladder.
Male genital examination is a physical examination of the genital in males to detect ailments and to assess sexual development, and is normally a component of an annual physical examination. The examination includes checking the penis, scrotum, and urethral meatus. A comprehensive assessment of the male genitals assesses the pubic hair based on Sexual Maturity Rating and the size of the testicles and penis. The exam can also be conducted to verify a person's age and biological sex. The genitourinary system can also be assessed as part of the male genital examination. During a genital examination, the doctor can detect any of the following: structural abnormalities, urethral opening abnormalities, problems related to not being circumcised, lumps, tumors, redness, excoriation, edema, lesions, swelling, cancer, hair-related issues, and many others. In some instances where a physical examination of the male genitals is not sufficient to diagnose an individual, then an internal genital examination using imaging or ultrasounds will be needed for further evaluation.

Warren Snodgrass is a pediatric urologist specializing in the repair of hypospadias, the second most common birth defect. In 1994 he described the tubularized incised plate (TIP) repair of hypospadias, which has become known as the Snodgrass repair and has become the most common approach to repairing most forms of hypospadias. Together with Dr. Nicol Bush, he also developed the STAG repair for severe hypospadias and the Snodbush repair used mainly for reoperations after unsuccessful surgery. Snodgrass is internationally known for his advocacy of evidence-based surgery, and was the editor of a textbook on pediatric urology. He is in private practice near Dallas, Texas.
Marc Goldstein, MD, DSc (hon), FACS is an American urologist and the Matthew P. Hardy Distinguished Professor of Reproductive Medicine, and Urology at Weill Cornell Medical College of Cornell University; Surgeon-in-Chief, Male Reproductive Medicine and Surgery; and Director of the Center of Male Reproductive Medicine and Microsurgery at the New York Presbyterian Hospital Weill Cornell Medical Center. He is Adjunct Senior Scientist with the Population Council's Center for Biomedical Research, located on the campus of Rockefeller University.