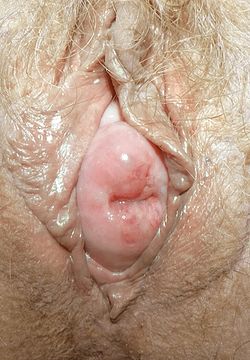
Vaginal prolapses are treated according to the severity of symptoms.
Non-surgical
With conservative measures, such as changes in diet and fitness, Kegel exercises, and pelvic floor physical therapy. [9]
A pessary, a rubber or silicone rubber device fitted to the patient is also a non-surgical option, it is inserted into the vagina and may be retained for up to several months. Vaginal pessaries can immediately relieve prolapse and prolapse-related symptoms. [10] Pessaries are a good choice of treatment for women who wish to maintain fertility, are poor surgical candidates, or who may not be able to attend physical therapy. [11] Pessaries require a provider to fit the device, but most can be removed, cleaned, and replaced by the woman herself; however, others have this done for them by a clinician biannually. A trial compared the two approaches and found that, compared with clinic-based care, self-management was associated with a similar quality of life, fewer complications, and was more cost-effective. [12] [13] Pessaries should be offered as a non-surgical alternative for women considering surgery.
Surgery
Surgery (for example native tissue repair, biological graft repair, absorbable and non-absorbable mesh repair, colpopexy, or colpocleisis) is used to treat symptoms such as bowel or urinary problems, pain, or a prolapse sensation. When operating a pelvic organ prolapse, introducing a mid-urethral sling during or after surgery seems to reduce stress urinary incontinence. [14] Transvaginal repair seems to be more effective than transanal repair in posterior wall prolapse, but adverse effects cannot be excluded. [15] According to the FDA, serious complications are "not rare." [16]
Evidence does not support the use of transvaginal surgical mesh compared with native tissue repair for anterior compartment prolapse owing to increased morbidity. [17] For posterior vaginal repair, the use of mesh or graft material does not seem to provide any benefits. [15]
Compared to native tissue repair, transvaginal permanent mesh likely reduces the perception of vaginal prolapse sensation, the risk of recurrent prolapse, and of having repeat surgery specifically only for prolapse. Transvaginal mesh (TVM) has a greater risk of bladder injury and of needing repeat surgery for stress urinary incontinence or mesh exposure. [18] The use of a TVM in treating vaginal prolapses is associated with severe side effects including organ perforation, infection, and pain.
Safety and efficacy of many newer meshes is unknown. [17] Thousands of class action lawsuits have been filed and settled against several manufacturers of TVM devices. [19]
For surgical treatment of apical vaginal prolapse, going through the abdomen (sacral colpopexy) may have better outcomes than a surgical approach that goes through the vagina. [6]