Related Research Articles

Fecal incontinence (FI), or in some forms, encopresis, is a lack of control over defecation, leading to involuntary loss of bowel contents — including flatus (gas), liquid stool elements and mucus, or solid feces. FI is a sign or a symptom, not a diagnosis. Incontinence can result from different causes and might occur with either constipation or diarrhea. Continence is maintained by several interrelated factors, including the anal sampling mechanism, and incontinence usually results from a deficiency of multiple mechanisms. The most common causes are thought to be immediate or delayed damage from childbirth, complications from prior anorectal surgery, altered bowel habits. An estimated 2.2% of community-dwelling adults are affected. However, reported prevalence figures vary. A prevalence of 8.39% among non-institutionalized U.S adults between 2005 and 2010 has been reported, and among institutionalized elders figures come close to 50%.

A rectal prolapse occurs when walls of the rectum have prolapsed to such a degree that they protrude out of the anus and are visible outside the body. However, most researchers agree that there are 3 to 5 different types of rectal prolapse, depending on whether the prolapsed section is visible externally, and whether the full or only partial thickness of the rectal wall is involved.

The pelvic floor or pelvic diaphragm is an anatomical location in the human body, which has an important role in urinary and anal continence, sexual function and support of the pelvic organs. The pelvic floor includes muscles, both skeletal and smooth, ligaments and fascia. and separates between the pelvic cavity from above, and the perineum from below. It is formed by the levator ani muscle and coccygeus muscle, and associated connective tissue.
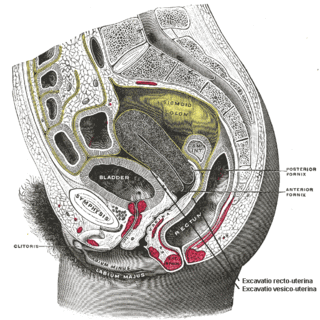
In gynecology, a rectocele or posterior vaginal wall prolapse results when the rectum bulges (herniates) into the vagina. Two common causes of this defect are childbirth and hysterectomy. Rectocele also tends to occur with other forms of pelvic organ prolapse, such as enterocele, sigmoidocele and cystocele.

Pelvic floor dysfunction is a term used for a variety of disorders that occur when pelvic floor muscles and ligaments are impaired. The condition affects up to 50 percent of women who have given birth. Although this condition predominantly affects women, up to 16 percent of men are affected as well. Symptoms can include pelvic pain, pressure, pain during sex, urinary incontinence (UI), overactive bladder, bowel incontinence, incomplete emptying of feces, constipation, myofascial pelvic pain and pelvic organ prolapse. When pelvic organ prolapse occurs, there may be visible organ protrusion or a lump felt in the vagina or anus. Research carried out in the UK has shown that symptoms can restrict everyday life for women. However, many people found it difficult to talk about it and to seek care, as they experienced embarrassment and stigma.

Colorectal surgery is a field in medicine dealing with disorders of the rectum, anus, and colon. The field is also known as proctology, but this term is now used infrequently within medicine and is most often employed to identify practices relating to the anus and rectum in particular. The word proctology is derived from the Greek words πρωκτός proktos, meaning "anus" or "hindparts", and -λογία -logia, meaning "science" or "study".
Colporrhaphy is a surgical procedure in women that repairs a defect in the wall of the vagina. It is the surgical intervention for both cystocele and rectocele.

Defecography is a type of medical radiological imaging in which the mechanics of a patient's defecation are visualized in real time using a fluoroscope. The anatomy and function of the anorectum and pelvic floor can be dynamically studied at various stages during defecation.

The rectum is the final straight portion of the large intestine in humans and some other mammals, and the gut in others. The adult human rectum is about 12 centimetres (4.7 in) long, and begins at the rectosigmoid junction at the level of the third sacral vertebra or the sacral promontory depending upon what definition is used. Its diameter is similar to that of the sigmoid colon at its commencement, but it is dilated near its termination, forming the rectal ampulla. It terminates at the level of the anorectal ring or the dentate line, again depending upon which definition is used. In humans, the rectum is followed by the anal canal, which is about 4 centimetres (1.6 in) long, before the gastrointestinal tract terminates at the anal verge. The word rectum comes from the Latin rēctumintestīnum, meaning straight intestine.

Humans mostly use one of two types of defecation postures to defecate: squatting and sitting. People use the squatting postures when using squat toilets or when defecating in the open in the absence of toilets. The sitting posture on the other hand is used in toilets that have a pedestal or "throne", where users generally lean forward or sit at 90 degrees to a toilet seat.

In humans, the anus is the external opening of the rectum located inside the intergluteal cleft. Two sphincters control the exit of feces from the body during an act of defecation, which is the primary function of the anus. These are the internal anal sphincter and the external anal sphincter, which are circular muscles that normally maintain constriction of the orifice and which relax as required by normal physiological functioning. The inner sphincter is involuntary and the outer is voluntary. Above the anus is the perineum, which is also located beneath the vulva or scrotum.
An enterocele is a herniation of a peritoneum-lined sac containing small intestine through the pelvic floor, between the rectum and the vagina. Enterocele is significantly more common in females, especially after hysterectomy.
Solitary rectal ulcer syndrome or SRUS is a chronic disorder of the rectal mucosa. It commonly occurs with varying degrees of rectal prolapse. The condition is thought to be caused by different factors, such as long term constipation, straining during defecation, and dyssynergic defecation. Treatment is by normalization of bowel habits, biofeedback, and other conservative measures. In more severe cases various surgical procedures may be indicated. The condition is relatively rare, affecting approximately 1 in 100,000 people per year. It affects mainly adults aged 30–50. Females are affected slightly more often than males. The disorder can be confused clinically with rectal cancer or other conditions such as inflammatory bowel disease, even when a biopsy is done.
Anismus or dyssynergic defecation is the failure of normal relaxation of pelvic floor muscles during attempted defecation. It can occur in both children and adults, and in both men and women. It can be caused by physical defects or it can occur for other reasons or unknown reasons. Anismus that has a behavioral cause could be viewed as having similarities with parcopresis, or psychogenic fecal retention.
Obstructed defecation syndrome is a major cause of functional constipation, of which it is considered a subtype. It is characterized by difficult and/or incomplete emptying of the rectum with or without an actual reduction in the number of bowel movements per week. Normal definitions of functional constipation include infrequent bowel movements and hard stools. In contrast, ODS may occur with frequent bowel movements and even with soft stools, and the colonic transit time may be normal, but delayed in the rectum and sigmoid colon.
Descending perineum syndrome refers to a condition where the perineum "balloons" several centimeters below the bony outlet of the pelvis during strain, although this descent may happen without straining. The syndrome was first described in 1966 by Parks et al.

Paolo Antonio Boccasanta is an Italian general surgeon, a professor at the University of Milan and a specialist in general, vascular and thoracic surgery. He took a qualification in Coloproctology in 2000 in Brighton (UK) from the European Board of Surgery.

The vaginal support structures are those muscles, bones, ligaments, tendons, membranes and fascia, of the pelvic floor that maintain the position of the vagina within the pelvic cavity and allow the normal functioning of the vagina and other reproductive structures in the female. Defects or injuries to these support structures in the pelvic floor leads to pelvic organ prolapse. Anatomical and congenital variations of vaginal support structures can predispose a woman to further dysfunction and prolapse later in life. The urethra is part of the anterior wall of the vagina and damage to the support structures there can lead to incontinence and urinary retention.
Ventral rectopexy is a surgical procedure for external rectal prolapse, internal rectal prolapse, and sometimes other conditions such as rectocele, obstructed defecation syndrome, or solitary rectal ulcer syndrome. The rectum is fixed into the desired position, usually using a biological or synthetic mesh which is attached to the sacral promontory. The effect of the procedure is correction of the abnormal descended position of the posterior compartment of the pelvis, reinforcement of the anterior (front) surface of the rectum, and elevation of the pelvic floor. In females, the rectal-vaginal septum is reinforced, and there is the opportunity to simultaneously correct any prolapse of the middle compartment. In such cases, ventral rectopexy may be combined with sacrocolpopexy. The surgery is usually performed laparoscopically.
A cul-de-sac hernia is a herniation of peritoneal folds into the rectovaginal septum, or the rectovesical septum. The herniated structure is the recto-uterine pouch in females, or the rectovesical pouch in males. The hernia descends below the proximal (upper) third of the vagina in females, or, according to another definition, below the pubococcygeal line (PCL).
References
- 1 2 3 4 5 6 7 Zbar, AP; Wexner, SD, eds. (18 March 2010). Coloproctology. Springer London. pp. 140–143. ISBN 978-1-84882-755-4.
- 1 2 3 4 5 6 7 8 9 Bordeianou LG, Carmichael JC, Paquette IM, Wexner S, Hull TL, Bernstein M, et al. (April 2018). "Consensus Statement of Definitions for Anorectal Physiology Testing and Pelvic Floor Terminology (Revised)" (PDF). Diseases of the Colon and Rectum. 61 (4): 421–427. doi:10.1097/DCR.0000000000001070. PMID 29521821.
- 1 2 3 Ratto C, Parrello A, Dionisi L, Litta F (2014). Coloproctology: Colon, Rectum and Anus: Anatomic, Physiologic and Diagnostic Bases for Disease Management. Cham, Switzerland: Springer International Publishing. pp. 229, 280. ISBN 978-3-319-10154-5.
- 1 2 3 Schlachta, CM; Sylla, P, eds. (2018). Current Common Dilemmas in Colorectal Surgery. Springer Nature. pp. 184, 186. doi:10.1007/978-3-319-70117-2. ISBN 978-3-319-70117-2.
- ↑ Steele SR, Maykel JA, Wexner SD (11 August 2020). Clinical Decision Making in Colorectal Surgery (2nd ed.). Cham: Springer International Publishing. pp. 22, 23. ISBN 978-3-319-65941-1.
- ↑ Brown, SR; Hartley, JE; Hill, J; Scott, N; Williams, G, eds. (2012). Contemporary Coloproctology. London Heidelberg: Springer. p. 391. ISBN 978-1-4471-5856-1.
- 1 2 3 4 Herold A, Lehur PA, Matzel KE, O'Connell PR (2017). European Manual of Medicine: Coloproctology (Second ed.). Berlin, Germany. pp. 9, 129. ISBN 978-3-662-53210-2.
{{cite book}}: CS1 maint: location missing publisher (link) - ↑ Schwandner, O; Poschenrieder, F; Gehl, HB; Bruch, HP (September 2004). "[Differential diagnosis in descending perineum syndrome]". Der Chirurg; Zeitschrift fur alle Gebiete der operativen Medizen. 75 (9): 850–60. doi:10.1007/s00104-004-0922-9. PMID 15258747.
- 1 2 Steele SR, Hull TL, Hyman N, Maykel JA, Read TE, Whitlow CB (20 November 2021). The ASCRS Textbook of Colon and Rectal Surgery (4th ed.). Cham, Switzerland: Springer Nature. p. 1014. ISBN 978-3-030-66049-9.