Related Research Articles

Bradycardia, also called bradyarrhythmia, is a resting heart rate under 60 beats per minute (BPM). While bradycardia can result from various pathologic processes, it is commonly a physiologic response to cardiovascular conditioning or due to asymptomatic type 1 atrioventricular block.

The heart is a muscular organ found in humans and other animals. This organ pumps blood through the blood vessels. Heart and blood vessels together make the circulatory system. The pumped blood carries oxygen and nutrients to the tissue, while carrying metabolic waste such as carbon dioxide to the lungs. In humans, the heart is approximately the size of a closed fist and is located between the lungs, in the middle compartment of the chest, called the mediastinum.

The parasympathetic nervous system (PSNS) is one of the three divisions of the autonomic nervous system, the others being the sympathetic nervous system and the enteric nervous system.
Baroreceptors are stretch receptors that sense blood pressure. Thus, increases in the pressure of blood vessel triggers increased action potential generation rates and provides information to the central nervous system. This sensory information is used primarily in autonomic reflexes that in turn influence the heart cardiac output and vascular smooth muscle to influence vascular resistance. Baroreceptors act immediately as part of a negative feedback system called the baroreflex, as soon as there is a change from the usual mean arterial blood pressure, returning the pressure toward a normal level. These reflexes help regulate short-term blood pressure. The solitary nucleus in the medulla oblongata of the brain recognizes changes in the firing rate of action potentials from the baroreceptors, and influences cardiac output and systemic vascular resistance.

Heart rate is the frequency of the heartbeat measured by the number of contractions of the heart per minute. The heart rate varies according to the body's physical needs, including the need to absorb oxygen and excrete carbon dioxide. It is also modulated by numerous factors, including genetics, physical fitness, stress or psychological status, diet, drugs, hormonal status, environment, and disease/illness, as well as the interaction between these factors. It is usually equal or close to the pulse rate measured at any peripheral point.
A cardiac function curve is a graph showing the relationship between right atrial pressure (x-axis) and cardiac output (y-axis). Superimposition of the cardiac function curve and venous return curve is used in one hemodynamic model.

The sinoatrial node is an oval shaped region of special cardiac muscle in the upper back wall of the right atrium made up of cells known as pacemaker cells. The sinus node is approximately 15 mm long, 3 mm wide, and 1 mm thick, located directly below and to the side of the superior vena cava.

The baroreflex or baroreceptor reflex is one of the body's homeostatic mechanisms that helps to maintain blood pressure at nearly constant levels. The baroreflex provides a rapid negative feedback loop in which an elevated blood pressure causes the heart rate to decrease. Decreased blood pressure decreases baroreflex activation and causes heart rate to increase and to restore blood pressure levels. Their function is to sense pressure changes by responding to change in the tension of the arterial wall. The baroreflex can begin to act in less than the duration of a cardiac cycle and thus baroreflex adjustments are key factors in dealing with postural hypotension, the tendency for blood pressure to decrease on standing due to gravity.

In human anatomy, the carotid sinus is a dilated area at the base of the internal carotid artery just superior to the bifurcation of the internal carotid and external carotid at the level of the superior border of thyroid cartilage. The carotid sinus extends from the bifurcation to the "true" internal carotid artery. The carotid sinuses are sensitive to pressure changes in the arterial blood at this level. They are two out of the four baroreception sites in humans and most mammals.
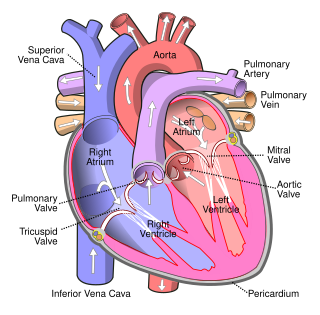
The atrium is one of the two upper chambers in the heart that receives blood from the circulatory system. The blood in the atria is pumped into the heart ventricles through the atrioventricular mitral and tricuspid heart valves.
Pulsus paradoxus, also paradoxic pulse or paradoxical pulse, is an abnormally large decrease in stroke volume, systolic blood pressure and pulse wave amplitude during inspiration. Pulsus paradoxus is not related to pulse rate or heart rate, and it is not a paradoxical rise in systolic pressure. Normally, blood pressure drops less precipitously than 10 mmHg during inhalation. Pulsus paradoxus is a sign that is indicative of several conditions, most commonly pericardial effusion.
The Hering–Breuer inflation reflex, named for Josef Breuer and Ewald Hering, is a reflex triggered to prevent the over-inflation of the lung. Pulmonary stretch receptors present on the wall of bronchi and bronchioles of the airways respond to excessive stretching of the lung during large inspirations.
Vagal tone is activity of the vagus nerve and a fundamental component of the parasympathetic branch of the autonomic nervous system. This branch of the nervous system is not under conscious control and is largely responsible for the regulation of several body compartments at rest. Vagal activity results in various effects, including: heart rate reduction, vasodilation/constriction of vessels, glandular activity in the heart, lungs, and digestive tract, liver, immune system regulation as well as control of gastrointestinal sensitivity, motility and inflammation.
Venous return is the rate of blood flow back to the heart. It normally limits cardiac output.
Reflex bradycardia is a bradycardia in response to the baroreceptor reflex, one of the body's homeostatic mechanisms for preventing abnormal increases in blood pressure. In the presence of high mean arterial pressure, the baroreceptor reflex produces a reflex bradycardia as a method of decreasing blood pressure by decreasing cardiac output.
The Bezold–Jarisch reflex involves a variety of cardiovascular and neurological processes which cause hypopnea, hypotension and bradycardia in response to noxious stimuli detected in the cardiac ventricles. The reflex is named after Albert von Bezold and Adolf Jarisch Junior. The significance of the discovery is that it was the first recognition of a chemical (non-mechanical) reflex.
The Nicoladoni–Branham sign is named after Carl Nicoladoni, who first noticed the phenomenon of the pulse slowing in a patient with right arm phlebarteriectasia when the brachialis artery proximal to it was compressed. In modern medicine, the sign is elicited when pressure is applied to an artery proximal to an arteriovenous fistula and said to be positive if the following occurs:

Pacemaker syndrome is a condition that represents the clinical consequences of suboptimal atrioventricular (AV) synchrony or AV dyssynchrony, regardless of the pacing mode, after pacemaker implantation. It is an iatrogenic disease—an adverse effect resulting from medical treatment—that is often underdiagnosed. In general, the symptoms of the syndrome are a combination of decreased cardiac output, loss of atrial contribution to ventricular filling, loss of total peripheral resistance response, and nonphysiologic pressure waves.
Low pressure baroreceptors or low pressure receptors are baroreceptors that relay information derived from blood pressure within the autonomic nervous system. They are stimulated by stretching of the vessel wall. They are located in large systemic veins and in the walls of the atria of the heart, and pulmonary vasculature. Low pressure baroreceptors are also referred to as volume receptors,cardiopulmonary baroreceptors, and veno-atrial stretch receptors
Cardiac physiology or heart function is the study of healthy, unimpaired function of the heart: involving blood flow; myocardium structure; the electrical conduction system of the heart; the cardiac cycle and cardiac output and how these interact and depend on one another.
References
- 1 2 3 4 Boron WF, Boulpaep EL, eds. (2017). Medical Physiology (3rd ed.). Philadelphia, PA: Elsevier. pp. 547–548. ISBN 978-1-4557-4377-3.
- 1 2 Crystal GJ, Salem MR (March 2012). "The Bainbridge and the "reverse" Bainbridge reflexes: history, physiology, and clinical relevance". Anesthesia and Analgesia. 114 (3): 520–532. doi:10.1213/ANE.0b013e3182312e21. PMID 21965361.
- 1 2 Pakkam ML, Moore MJ (2024). "Physiology, Bainbridge Reflex". StatPearls. Treasure Island (FL): StatPearls Publishing. PMID 31082061 . Retrieved 2024-12-12.
- ↑ Mortola JP, Marghescu D, Siegrist-Johnstone R (April 2015). "Respiratory sinus arrhythmia in young men and women at different chest wall configurations". Clinical Science. 128 (8): 507–516. doi:10.1042/CS20140543. PMID 25387977.
- ↑ Hakumäki MO (June 1987). "Seventy years of the Bainbridge reflex". Acta Physiologica Scandinavica. 130 (2): 177–185. doi:10.1111/j.1748-1716.1987.tb08126.x. PMID 3300168.
- ↑ Bainbridge FA (December 1915). "The influence of venous filling upon the rate of the heart". The Journal of Physiology. 50 (2): 65–84. doi:10.1113/jphysiol.1915.sp001736. PMC 1420590 . PMID 16993330.
- 1 2 3 4 Hall JE, Hall ME, Guyton AC (2021). Guyton and Hall Textbook of Medical Physiology (14th ed.). Philadelphia, PA: Elsevier. pp. 224–225. ISBN 978-0-323-59712-8.
- ↑ Jones JJ (February 1962). "The Bainbridge reflex". The Journal of Physiology. 160 (2): 298–305. doi:10.1113/jphysiol.1962.sp006847. PMC 1359533 . PMID 14452295.
- ↑ Coleridge JC, Linden RJ (May 1955). "The effect of intravenous infusions upon the heart rate of the anaesthetized dog". The Journal of Physiology. 128 (2): 310–319. doi:10.1113/jphysiol.1955.sp005308. PMC 1365860 . PMID 14392610.
- ↑ Salah HM, Gupta R, Hicks AJ, Mahmood K, Haglund NA, Bindra AS, et al. (September 2024). "Baroreflex Function in Cardiovascular Disease". Journal of Cardiac Failure. doi: 10.1016/j.cardfail.2024.08.062 . PMID 39341547.
- ↑ Campagna JA, Carter C (May 2003). "Clinical relevance of the Bezold-Jarisch reflex". Anesthesiology. 98 (5): 1250–1260. doi:10.1097/00000542-200305000-00030. PMID 12717149.
- ↑ Hennis K, Piantoni C, Biel M, Fenske S, Wahl-Schott C (May 2024). "Pacemaker Channels and the Chronotropic Response in Health and Disease". Circulation Research. 134 (10): 1348–1378. doi:10.1161/CIRCRESAHA.123.323250. PMC 11081487 . PMID 38723033.
- 1 2 3 4 Koeppen BM, Stanton BA, Swiatecka-Urban A, eds. (2024). Berne & Levy Physiology (8th ed.). Philadelphia, PA: Elsevier. ISBN 978-0-323-84790-2.
- ↑ Hakumäki MO (1987). "Seventy years of the Bainbridge reflex". Acta Physiologica Scandinavica. 130 (2): 177–185. doi:10.1111/j.1748-1716.1987.tb08126.x. ISSN 1365-201X.
- ↑ Reitz BA, Dong E, Stinson EB (May 1971). "The Bainbridge reflex in canine cardiac autotransplants". Circulation. 43 (5 Supplement 1): I136 –I140. doi:10.1161/01.CIR.43.5S1.I-136. PMID 4931289.
- ↑ Reitz BA, Dong E, Stinson EB (May 1971). "The Bainbridge Reflex in Canine Cardiac Autotransplants". Circulation. 43 (5 Supplement 1): I–I136. doi:10.1161/01.CIR.43.5S1.I-136.
- ↑ Mohanty PK, Thames MD, Arrowood JA, Sowers JR, McNamara C, Szentpetery S (May 1987). "Impairment of cardiopulmonary baroreflex after cardiac transplantation in humans". Circulation. 75 (5): 914–921. doi:10.1161/01.CIR.75.5.914.
- ↑ Quinn TA, Kohl P (2022). "The Bainbridge effect: stretching our understanding of cardiac pacemaking for more than a century". The Journal of Physiology. 600 (20): 4377–4379. doi: 10.1113/JP283610 . ISSN 1469-7793.
- ↑ Cooper PJ, Lei M, Cheng LX, Kohl P (November 2000). "Selected contribution: axial stretch increases spontaneous pacemaker activity in rabbit isolated sinoatrial node cells". Journal of Applied Physiology. 89 (5). Bethesda, Md.: 2099–104. doi:10.1152/jappl.2000.89.5.2099. PMID 11053369.
- ↑ Rossberg F (September 1973). "[The Bainbridge effect]". Zeitschrift Fur Die Gesamte Innere Medizin Und Ihre Grenzgebiete (in German). 28 (17): 513–8. PMID 4588170.