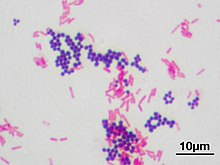
Antimicrobial resistance (AMR) occurs when microbes evolve mechanisms that protect them from the effects of antimicrobials. Antibiotic resistance is a subset of AMR, that applies specifically to bacteria that become resistant to antibiotics.

Ciprofloxacin is a fluoroquinolone antibiotic used to treat a number of bacterial infections. This includes bone and joint infections, intra abdominal infections, certain type of infectious diarrhea, respiratory tract infections, skin infections, typhoid fever, and urinary tract infections, among others. For some infections it is used in addition to other antibiotics. It can be taken by mouth, as eye drops, as ear drops, or intravenously.

Neurology is a branch of medicine dealing with disorders of the nervous system. Neurology deals with the diagnosis and treatment of all categories of conditions and disease involving the central and peripheral nervous systems, including their coverings, blood vessels, and all effector tissue, such as muscle. Neurological practice relies heavily on the field of neuroscience, the scientific study of the nervous system.

An infection is the invasion of an organism's body tissues by disease-causing agents, their multiplication, and the reaction of host tissues to the infectious agents and the toxins they produce. An infectious disease, also known as a transmissible disease or communicable disease, is an illness resulting from an infection.
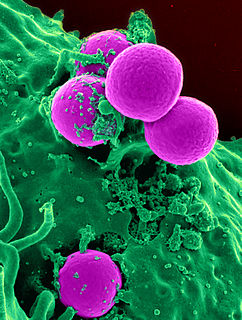
Methicillin-resistant Staphylococcus aureus (MRSA) is a group of Gram-positive bacteria that are genetically distinct from other strains of Staphylococcus aureus. MRSA is responsible for several difficult-to-treat infections in humans. It caused more than 100,000 deaths attributable to antimicrobial resistance in 2019.
Internal medicine or general internal medicine is the medical specialty dealing with the prevention, diagnosis, and treatment of internal diseases. Physicians specializing in internal medicine are called internists, or physicians in Commonwealth nations. Internists are skilled in the management of patients who have undifferentiated or multi-system disease processes. Internists care for hospitalized and ambulatory patients and may play a major role in teaching and research. Internal medicine and family medicine are often confused as equivalent in the Commonwealth nations.
Bloodstream infections (BSIs), which include bacteremias when the infections are bacterial and fungemias when the infections are fungal, are infections present in the blood. Blood is normally a sterile environment, so the detection of microbes in the blood is always abnormal. A bloodstream infection is different from sepsis, which is the host response to bacteria.

Klebsiella pneumoniae is a Gram-negative, non-motile, encapsulated, lactose-fermenting, facultative anaerobic, rod-shaped bacterium. It appears as a mucoid lactose fermenter on MacConkey agar.

Pulmonology, pneumology or pneumonology is a medical specialty that deals with diseases involving the respiratory tract. It is also known as respirology, respiratory medicine, or chest medicine in some countries and areas.

Tropical medicine is an interdisciplinary branch of medicine that deals with health issues that occur uniquely, are more widespread, or are more difficult to control in tropical and subtropical regions.
Infection prevention and control is the discipline concerned with preventing healthcare-infections; a practical rather than academic sub-discipline of epidemiology. In Northern Europe, infection prevention and control is expanded from healthcare into a component in public health, known as "infection protection". It is an essential part of the infrastructure of health care. Infection control and hospital epidemiology are akin to public health practice, practiced within the confines of a particular health-care delivery system rather than directed at society as a whole.
Internal medicine-pediatrics, or med-peds, is a medical specialty in which doctors train to be board certified in both internal medicine and pediatrics. A residency program in med-peds is four years in length, contrasted with three years for internal medicine or pediatrics alone. Upon completion of a med-peds residency, a doctor can practice in the areas of internal medicine, pediatrics or can complete a fellowship program to further specialize in an internal medicine or pediatrics sub-field.
Adolescent medicine also known as adolescent and young adult medicine is a medical subspecialty that focuses on care of patients who are in the adolescent period of development. This period begins at puberty and lasts until growth has stopped, at which time adulthood begins. Typically, patients in this age range will be in the last years of middle school up until college graduation. In developed nations, the psychosocial period of adolescence is extended both by an earlier start, as the onset of puberty begins earlier, and a later end, as patients require more years of education or training before they reach economic independence from their parents.

The Infectious Diseases Society of America (IDSA) is a medical association representing physicians, scientists and other health care professionals who specialize in infectious diseases. It was founded in 1963 and is based in Arlington, Virginia. As of 2018 IDSA had more than 11,000 members from across the United States and nearly 100 other countries on six different continents. IDSA's purpose is to improve the health of individuals, communities, and society by promoting excellence in patient care, education, research, public health, and prevention relating to infectious diseases. It is a 501(c)(6) organization.

Medical microbiology, the large subset of microbiology that is applied to medicine, is a branch of medical science concerned with the prevention, diagnosis and treatment of infectious diseases. In addition, this field of science studies various clinical applications of microbes for the improvement of health. There are four kinds of microorganisms that cause infectious disease: bacteria, fungi, parasites and viruses, and one type of infectious protein called prion.

Antibiotic misuse, sometimes called antibiotic abuse or antibiotic overuse, refers to the misuse or overuse of antibiotics, with potentially serious effects on health. It is a contributing factor to the development of antibiotic resistance, including the creation of multidrug-resistant bacteria, informally called "super bugs": relatively harmless bacteria can develop resistance to multiple antibiotics and cause life-threatening infections.
Antimicrobial stewardship is the systematic effort to educate and persuade prescribers of antimicrobials to follow evidence-based prescribing, in order to stem antibiotic overuse, and thus antimicrobial resistance. AMS has been an organized effort of specialists in infectious diseases, both in Internal Medicine and Pediatrics with their respective peer-organizations, hospital pharmacists, the public health community and their professional organizations since the late 1990s. It has first been implemented in hospitals. In the U.S., within the context of physicians' prescribing freedom, AMS had largely been voluntary self-regulation in the form of policies and appeals to adhere to a prescribing self-discipline until 2017, when the Joint Commission prescribed that hospitals should have an Antimicrobial Stewardship team, which was expanded to the outpatient setting in 2020.
The Society of Infectious Diseases Pharmacists (SIDP) is a non-profit professional association of pharmacists and allied health professionals who specialize in infectious diseases and antimicrobial stewardship. According to the Board of Pharmaceutical Specialties, clinical pharmacists specializing in infectious diseases are trained in the use of microbiology and pharmacology to develop, implement, and monitor drug regimens that incorporate the pharmacodynamics and pharmacokinetics of antimicrobials for patients.
Jasmine R. Marcelin is a Caribbean-American infectious disease physician and an Assistant Professor in the Department of Internal Medicine at the University of Nebraska Medical Center (UNMC). Marcelin is also the Associate Medical Director of the Antimicrobial Stewardship Program and as well as the Co-Director of Digital Innovation and Social Media Strategy at UNMC. Marcelin is dedicated to advancing diversity, inclusion, and equity in her communities and is a founding member of the Infectious Diseases Society of America Inclusion, Diversity, Access & Equity Taskforce. Marcelin uses social media to advance medicine, diversity, and patient advocacy and has published articles on how to effectively use social media for these purposes.