
Medicare is an unofficial designation used to refer to the publicly funded single-payer healthcare system of Canada. Canada's health care system consists of 13 provincial and territorial health insurance plans, which provide universal healthcare coverage to Canadian citizens, permanent residents, and depending on the province or territory, certain temporary residents. The systems are individually administered on a provincial or territorial basis, within guidelines set by the federal government. The formal terminology for the insurance system is provided by the Canada Health Act and the health insurance legislation of the individual provinces and territories.

Health care, or healthcare, is the improvement of health via the prevention, diagnosis, treatment, amelioration or cure of disease, illness, injury, and other physical and mental impairments in people. Health care is delivered by health professionals and allied health fields. Medicine, dentistry, pharmacy, midwifery, nursing, optometry, audiology, psychology, occupational therapy, physical therapy, athletic training, and other health professions all constitute health care. The term includes work done in providing primary care, secondary care, tertiary care, and public health.

The healthcare industry is an aggregation and integration of sectors within the economic system that provides goods and services to treat patients with curative, preventive, rehabilitative, and palliative care. It encompasses the creation and commercialization of products and services conducive to the preservation and restoration of well-being. The contemporary healthcare sector comprises three fundamental facets, namely services, products, and finance. It can be further subdivided into numerous sectors and categories and relies on interdisciplinary teams of highly skilled professionals and paraprofessionals to address the healthcare requirements of both individuals and communities.

The Canada Health Act, adopted in 1984, is the federal legislation in Canada for publicly-funded health insurance, commonly called "medicare", and sets out the primary objective of Canadian healthcare policy.
Health insurance or medical insurance is a type of insurance that covers the whole or a part of the risk of a person incurring medical expenses. As with other types of insurance, risk is shared among many individuals. By estimating the overall risk of health risk and health system expenses over the risk pool, an insurer can develop a routine finance structure, such as a monthly premium or payroll tax, to provide the money to pay for the health care benefits specified in the insurance agreement. The benefit is administered by a central organization, such as a government agency, private business, or not-for-profit entity.

A comparison of the healthcare systems in Canada and the United States is often made by government, public health and public policy analysts. The two countries had similar healthcare systems before Canada changed its system in the 1960s and 1970s. The United States spends much more money on healthcare than Canada, on both a per-capita basis and as a percentage of GDP. In 2006, per-capita spending for health care in Canada was US$3,678; in the U.S., US$6,714. The U.S. spent 15.3% of GDP on healthcare in that year; Canada spent 10.0%. In 2006, 70% of healthcare spending in Canada was financed by government, versus 46% in the United States. Total government spending per capita in the U.S. on healthcare was 23% higher than Canadian government spending. U.S. government expenditure on healthcare was just under 83% of total Canadian spending.

Healthcare in Canada is delivered through the provincial and territorial systems of publicly funded health care, informally called Medicare. It is guided by the provisions of the Canada Health Act of 1984, and is universal. The 2002 Royal Commission, known as the Romanow Report, revealed that Canadians consider universal access to publicly funded health services as a "fundamental value that ensures national health care insurance for everyone wherever they live in the country".
Health care in Ireland is delivered through public and private healthcare. The public health care system is governed by the Health Act 2004, which established a new body to be responsible for providing health and personal social services to everyone living in Ireland – the Health Service Executive. The new national health service came into being officially on 1 January 2005; however the new structures are currently in the process of being established as the reform programme continues. In addition to the public-sector, there is also a large private healthcare market.
The prices of health care in the United States are higher than in other countries. Compared to other OECD countries, U.S. healthcare costs are one-third higher or more relative to the size of the economy (GDP). According to the CDC, during 2015, health expenditures per-person were nearly $10,000 on average, with total expenditures of $3.2 trillion or 17.8% of GDP. Proximate reasons for the differences with other countries include higher prices for the same services and greater use of healthcare. Higher administrative costs, higher per-capita income, and less government intervention to drive down prices are deeper causes. While the annual inflation rate in healthcare costs has declined in recent decades, it still remains above the rate of economic growth, resulting in a steady increase in healthcare expenditures relative to GDP from 6% in 1970 to nearly 18% in 2015.

The Swedish health care system is mainly government-funded, universal for all citizens and decentralized, although private health care also exists. The health care system in Sweden is financed primarily through taxes levied by county councils and municipalities. A total of 21 councils are in charge with primary and hospital care within the country.
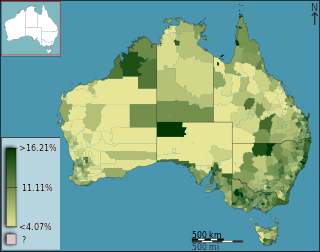
Health care in Australia operates under a shared public-private model underpinned by the Medicare system, the national single-payer funding model. State and territory governments operate public health facilities where eligible patients receive care free of charge. Primary health services, such as GP clinics, are privately owned in most situations, but attract Medicare rebates. Australian citizens, permanent residents, and some visitors and visa holders are eligible for health services under the Medicare system. Individuals are encouraged through tax surcharges to purchase health insurance to cover services offered in the private sector, and further fund health care.

Germany has a universal multi-payer health care system paid for by a combination of statutory health insurance and private health insurance.

Healthcare in Turkey consists of a mix of public and private health services. Turkey introduced universal health care in 2003. Known as Universal Health Insurance Genel Sağlık Sigortası, it is funded by a tax surcharge on employers, currently at 5%. Public-sector funding covers approximately 75.2% of health expenditures.
Healthcare in Finland consists of a highly decentralized three-level publicly funded healthcare system and a much smaller private sector. Although the Ministry of Social Affairs and Health has the highest decision-making authority, specific healthcare precincts are responsible for providing healthcare to their residents as of 2023.

Healthcare in Denmark is largely provided by the local governments of the five regions, with coordination and regulation by central government, while nursing homes, home care, and school health services are the responsibility of the 98 municipalities. Some specialised hospital services are managed centrally.

In the United States, healthcare is largely provided by private sector healthcare facilities, and paid for by a combination of public programs, private insurance, and out-of-pocket payments. The U.S. is the only developed country without a system of universal healthcare, and a significant proportion of its population lacks health insurance. The United States spends more on healthcare than any other country, both in absolute terms and as a percentage of GDP; however, this expenditure does not necessarily translate into better overall health outcomes compared to other developed nations. Coverage varies widely across the population, with certain groups, such as the elderly and low-income individuals, receiving more comprehensive care through government programs such as Medicaid and Medicare.

Examples of health care systems of the world, sorted by continent, are as follows.
Government-guaranteed health care for all citizens of a country, often called universal health care, is a broad concept that has been implemented in several ways. The common denominator for all such programs is some form of government action aimed at broadly extending access to health care and setting minimum standards. Most implement universal health care through legislation, regulation, and taxation. Legislation and regulation direct what care must be provided, to whom, and on what basis.
Health care finance in the United States discusses how Americans obtain and pay for their healthcare, and why U.S. healthcare costs are the highest in the world based on various measures.

Healthcare in Slovakia has features of the Bismarck, the Beveridge and the National health insurance systems. It has public health system paid largely from taxation. The cost of national health insurance is shared between the employees and the employers. The part of these taxes are paid by the employees as a deduction from theirs wages and the remaining part of these taxes is paid as compulsory contribution by employers. Sole traders pay the full amount of these taxes.













