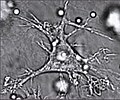
| Dendritic cell | |
|---|---|
 Dendritic cells in skin | |
 Artistic rendering of the surface of a human dendritic cell illustrating sheet-like processes that fold back onto the membrane surface. | |
| Details | |
| System | Immune system |
| Identifiers | |
| Latin | cellula dendritiformis |
| MeSH | D003713 |
| TH | H1.00.01.0.00038 |
| FMA | 83036 |
| Anatomical terminology | |
A dendritic cell (DC) is an antigen-presenting cell (also known as an accessory cell) of the mammalian immune system. A DC's main function is to process antigen material and present it on the cell surface to the T cells of the immune system. They act as messengers between the innate and adaptive immune systems. [1]
Contents
- History
- Types
- In vivo – primate
- In blood
- In vitro
- Development and life cycle
- Formation of immature cells and their maturation
- Life span
- Research challenges
- Cytokines
- Disease
- Blastic plasmacytoid dendritic cell neoplasm
- Viral infection
- Cancer
- Autoimmunity
- Other animals
- Media
- See also
- References
- External links
Dendritic cells are present in tissues that are in contact with the body's external environment, such as the skin, and the inner lining of the nose, lungs, stomach and intestines. They can also be found in an immature and mature state in the blood. Once activated, they migrate to the lymph nodes, where they interact with T cells and B cells to initiate and shape the adaptive immune response. At certain development stages they grow branched projections, the dendrites, that give the cell its name (δένδρον or déndron being Greek for 'tree'). While similar in appearance to the dendrites of neurons, these are structures distinct from them. Immature dendritic cells are also called veiled cells, as they possess large cytoplasmic 'veils' rather than dendrites.[ citation needed ]