
Foix–Alajouanine syndrome, also called subacute ascending necrotizing myelitis, is a disease caused by an arteriovenous malformation of the spinal cord. In particular, most cases involve dural arteriovenous malformations that present in the lower thoracic or lumbar spinal cord. The condition is named after Charles Foix and Théophile Alajouanine who first described the condition in 1926.

Syringomyelia is a generic term referring to a disorder in which a cyst or cavity forms within the spinal cord. Often, syringomyelia is used as a generic term before an etiology is determined. This cyst, called a syrinx, can expand and elongate over time, destroying the spinal cord. The damage may result in loss of feeling, paralysis, weakness, and stiffness in the back, shoulders, and extremities. Syringomyelia may also cause a loss of the ability to feel extremes of hot or cold, especially in the hands. It may also lead to a cape-like bilateral loss of pain and temperature sensation along the upper chest and arms. The combination of symptoms varies from one patient to another depending on the location of the syrinx within the spinal cord, as well as its extent.

Spina bifida /ˌspaɪnə ˈbɪfɪdə/ is a birth defect in which there is incomplete closing of the spine and the membranes around the spinal cord during early development in pregnancy. There are three main types: spina bifida occulta, meningocele and myelomeningocele. Meningocele and myelomeningocele may be grouped as spina bifida cystica. The most common location is the lower back, but in rare cases it may be in the middle back or neck.

Chiari malformation (CM) is a structural defect in the cerebellum, characterized by a downward displacement of one or both cerebellar tonsils through the foramen magnum. CMs can cause headaches, difficulty swallowing, vomiting, dizziness, neck pain, unsteady gait, poor hand coordination, numbness and tingling of the hands and feet, and speech problems. Less often, people may experience ringing or buzzing in the ears, weakness, slow heart rhythm, or fast heart rhythm, curvature of the spine (scoliosis) related to spinal cord impairment, abnormal breathing, such as central sleep apnea, characterized by periods of breathing cessation during sleep, and, in severe cases, paralysis.
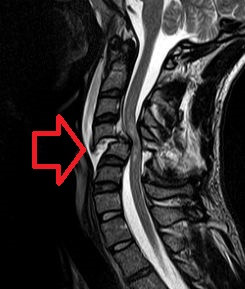
A spinal cord injury (SCI) is damage to the spinal cord that causes temporary or permanent changes in its function. Symptoms may include loss of muscle function, sensation, or autonomic function in the parts of the body served by the spinal cord below the level of the injury. Injury can occur at any level of the spinal cord and can be complete, with a total loss of sensation and muscle function at lower sacral segments, or incomplete, meaning some nervous signals are able to travel past the injured area of the cord up to the Sacral S4-5 spinal cord segments. Depending on the location and severity of damage, the symptoms vary, from numbness to paralysis, including bowel or bladder incontinence. Long term outcomes also range widely, from full recovery to permanent tetraplegia or paraplegia. Complications can include muscle atrophy, loss of voluntary motor control, spasticity, pressure sores, infections, and breathing problems.

Arachnoiditis is an inflammatory condition of the arachnoid mater or 'arachnoid', one of the membranes known as meninges that surround and protect the central nervous system. The outermost layer of the meninges is the dura mater and adheres to inner surface of the skull and vertebrae. The arachnoid is under or "deep" to the dura and is a thin membrane that adheres directly to the surface of the brain and spinal cord.

Cauda equina syndrome (CES) is a condition that occurs when the bundle of nerves below the end of the spinal cord known as the cauda equina is damaged. Signs and symptoms include low back pain, pain that radiates down the leg, numbness around the anus, and loss of bowel or bladder control. Onset may be rapid or gradual.

The conus medullaris or conus terminalis is the tapered, lower end of the spinal cord. It occurs near lumbar vertebral levels 1 (L1) and 2 (L2), occasionally lower. The upper end of the conus medullaris is usually not well defined, however, its corresponding spinal cord segments are usually S1–S5.

The central canal is the cerebrospinal fluid-filled space that runs through the spinal cord. The central canal lies below and is connected to the ventricular system of the brain, from which it receives cerebrospinal fluid, and shares the same ependymal lining. The central canal helps to transport nutrients to the spinal cord as well as protect it by cushioning the impact of a force when the spine is affected.

Kyphoscoliosis describes an abnormal curvature of the spine in both the coronal and sagittal planes. It is a combination of kyphosis and scoliosis. This musculoskeletal disorder often leads to other issues in patients, such as under-ventilation of lungs, pulmonary hypertension, difficulty in performing day-to-day activities, psychological issues emanating from anxiety about acceptance among peers, especially in young patients. It can also be seen in syringomyelia, Friedreich's ataxia, spina bifida, kyphoscoliotic Ehlers–Danlos syndrome (kEDS), and Duchenne muscular dystrophy due to asymmetric weakening of the paraspinal muscles.
Neurogenic bladder dysfunction, often called by the shortened term neurogenic bladder, refers to urinary bladder problems due to disease or injury of the central nervous system or peripheral nerves involved in the control of urination. There are multiple types of neurogenic bladder depending on the underlying cause and the symptoms. Symptoms include overactive bladder, urinary urgency, frequency, incontinence or difficulty passing urine. A range of diseases or conditions can cause neurogenic bladder including spinal cord injury, multiple sclerosis, stroke, brain injury, spina bifida, peripheral nerve damage, Parkinson's disease, or other neurodegenerative diseases. Neurogenic bladder can be diagnosed through a history and physical as well as imaging and more specialized testing. In addition to symptomatic treatment, treatment depends on the nature of the underlying disease and can be managed with behavioral changes, medications, surgeries, or other procedures. The symptoms of neurogenic bladder, especially incontinence, can severely degrade a person's quality of life.

Central cord syndrome (CCS) is the most common form of cervical spinal cord injury. It is characterized by loss of power and sensation in arms and hands. It usually results from trauma which causes damage to the neck, leading to major injury to the central corticospinal tract of the spinal cord. CCS most frequently occurs among older persons with cervical spondylosis, however, it also may occur in younger individuals.

Diastematomyelia is a congenital disorder in which a part of the spinal cord is split, usually at the level of the upper lumbar vertebra in the longitudinal (sagittal) direction. Females are affected much more commonly than males. This condition occurs in the presence of an osseous, cartilaginous or fibrous septum in the central portion of the spinal canal which then produces a complete or incomplete sagittal division of the spinal cord into two hemicords. When the split does not reunite distally to the spur, the condition is referred to as diplomyelia, which is true duplication of the spinal cord.
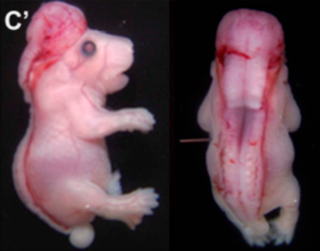
Rachischisis is a developmental birth defect involving the neural tube. This anomaly occurs in utero, when the posterior neuropore of the neural tube fails to close by the 27th intrauterine day. As a consequence the vertebrae overlying the open portion of the spinal cord do not fully form and remain unfused and open, leaving the spinal cord exposed. Patients with rachischisis have motor and sensory deficits, chronic infections, and disturbances in bladder function. This defect often occurs with anencephaly.

Spinal disease refers to a condition impairing the backbone. These include various diseases of the back or spine ("dorso-"), such as kyphosis. Dorsalgia refers to back pain. Some other spinal diseases include spinal muscular atrophy, ankylosing spondylitis, lumbar spinal stenosis, spina bifida, spinal tumors, osteoporosis and cauda equina syndrome.
Karin Marie Muraszko is an American pediatric neurosurgeon.

Nicholas Theodore is an American neurosurgeon and researcher at Johns Hopkins University School of Medicine. He is known for his work in spinal trauma, minimally invasive surgery, robotics, and personalized medicine. He is Director of the Neurosurgical Spine Program at Johns Hopkins and Co-Director of the Carnegie Center for Surgical Innovation at Johns Hopkins.

Cervicocranial syndrome or is a neurological illness. It is a combination of symptoms that are caused by an abnormality in the neck. The bones of the neck that are affected are cervical vertebrae (C1-C7). This syndrome can be identified by confirming cervical bone shifts, collapsed cervical bones or misalignment of the cervical bone leading to improper functioning of cervical spinal nerves. Cervicocranial syndrome is either congenital or acquired. Some examples of diseases that could result in cervicocranial syndrome are Chiari disease, Klippel-Feil malformation osteoarthritis, and trauma. Treatment options include neck braces, pain medication and surgery. The quality of life for individuals suffering from CCJ syndrome can improve through surgery.
Caudal duplication, is a rare congenital disorder in which various structures of the caudal region, embryonic cloaca, and neural tube exhibit a spectrum of abnormalities such as duplication and malformations. The exact causes of the condition is unknown, though there are several theories implicating abnormal embryological development as a cause for the condition. Diagnosis is often made during prenatal development of the second trimester through anomaly scans or immediately after birth. However, rare cases of adulthood diagnosis has also been observed. Treatment is often required to correct such abnormalities according to the range of symptoms present, whilst treatment options vary from conservative expectant management to resection of caudal tissue to restore normal function or appearance. As a rare congenital disorder, the prevalence at birth is less than 1 per 100,000 with less than 100 cases reported worldwide.
A lipomyelomeningocele is a type of closed neural tube defect that affects around 3 to 6 babies out of 100,000 births. It is an example of a spinal lipoma, which is a collection of adipose tissue, or fat, that is located at or around the spinal cord. Essentially, it is a tumor of fat located on the spinal cord. A lipomyelomeningocele defect is present at birth and can present with physical defect of the spine and back, and it can also cause various neurological symptoms such as weakness and bladder and bowel incontinence. The general treatment for this spinal defect is surgical detachment of the lipoma from the spine.















