Related Research Articles

Borderline personality disorder (BPD) is a personality disorder characterized by a pervasive, long-term pattern of significant interpersonal relationship instability, a distorted sense of self, and intense emotional responses. People diagnosed with BPD frequently exhibit self-harming behaviours and engage in risky activities, primarily due to challenges regulating emotional states to a healthy, stable baseline. Symptoms such as dissociation, a pervasive sense of emptiness, and an acute fear of abandonment are prevalent among those affected.

A mood swing is an extreme or sudden change of mood. Such changes can play a positive or a disruptive part in promoting problem solving and in producing flexible forward planning. When mood swings are severe, they may be categorized as part of a mental illness, such as bipolar disorder, where erratic and disruptive mood swings are a defining feature.
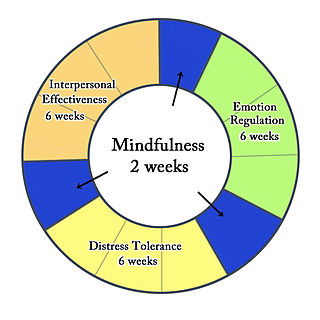
Dialectical behavior therapy (DBT) is an evidence-based psychotherapy that began with efforts to treat personality disorders and interpersonal conflicts. Evidence suggests that DBT can be useful in treating mood disorders and suicidal ideation as well as for changing behavioral patterns such as self-harm and substance use. DBT evolved into a process in which the therapist and client work with acceptance and change-oriented strategies and ultimately balance and synthesize them—comparable to the philosophical dialectical process of thesis and antithesis, followed by synthesis.
Child psychopathology refers to the scientific study of mental disorders in children and adolescents. Oppositional defiant disorder, attention-deficit hyperactivity disorder, and autism spectrum disorder are examples of psychopathology that are typically first diagnosed during childhood. Mental health providers who work with children and adolescents are informed by research in developmental psychology, clinical child psychology, and family systems. Lists of child and adult mental disorders can be found in the International Statistical Classification of Diseases and Related Health Problems, 10th Edition (ICD-10), published by the World Health Organization (WHO) and in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), published by the American Psychiatric Association (APA). In addition, the Diagnostic Classification of Mental Health and Developmental Disorders of Infancy and Early Childhood is used in assessing mental health and developmental disorders in children up to age five.
Irritability is the excitatory ability that living organisms have to respond to changes in their environment. The term is used for both the physiological reaction to stimuli and for the pathological, abnormal or excessive sensitivity to stimuli.
Reduced affect display, sometimes referred to as emotional blunting or emotional numbing, is a condition of reduced emotional reactivity in an individual. It manifests as a failure to express feelings either verbally or nonverbally, especially when talking about issues that would normally be expected to engage emotions. In this condition, expressive gestures are rare and there is little animation in facial expression or vocal inflection. Additionally, reduced affect can be symptomatic of autism, schizophrenia, depression, post-traumatic stress disorder, depersonalization-derealization disorder, schizoid personality disorder or brain damage. It may also be a side effect of certain medications.

In psychology, emotional detachment, also known as emotional blunting, is a condition or state in which a person lacks emotional connectivity to others, whether due to an unwanted circumstance or as a positive means to cope with anxiety. Such a coping strategy, also known as emotion-focused coping, is used when avoiding certain situations that might trigger anxiety. It refers to the evasion of emotional connections. Emotional detachment may be a temporary reaction to a stressful situation, or a chronic condition such as depersonalization-derealization disorder. It may also be caused by certain antidepressants. Emotional blunting, also known as reduced affect display, is one of the negative symptoms of schizophrenia.
Emotional dysregulation is characterized by an inability to flexibly respond to and manage emotional states, resulting in intense and prolonged emotional reactions that deviate from social norms, given the nature of the environmental stimuli encountered. Such reactions not only deviate from accepted social norms but also surpass what is informally deemed appropriate or proportional to the encountered stimuli.
Hysteroid dysphoria is a name given to repeated episodes of depressed mood in response to feeling rejected.
Neuroticism is a personality trait associated with negative emotions. It is one of the Big Five traits. Individuals with high scores on neuroticism are more likely than average to experience such feelings as anxiety, worry, fear, anger, frustration, envy, jealousy, pessimism, guilt, depressed mood, and loneliness. Such people are thought to respond worse to stressors and are more likely to interpret ordinary situations, such as minor frustrations, as appearing hopelessly difficult. Their behavioral responses may include procrastination, substance use, and other maladaptive behaviors, which may temporarily aid in relieving negative emotions and generating positive ones.

Bipolar disorder in children, or pediatric bipolar disorder (PBD), is a rare mental disorder in children and adolescents. The diagnosis of bipolar disorder in children has been heavily debated for many reasons including the potential harmful effects of adult bipolar medication use for children. PBD is similar to bipolar disorder (BD) in adults, and has been proposed as an explanation for periods of extreme shifts in mood called mood episodes. These shifts alternate between periods of depressed or irritable moods and periods of abnormally elevated moods called manic or hypomanic episodes. Mixed mood episodes can occur when a child or adolescent with PBD experiences depressive and manic symptoms simultaneously. Mood episodes of children and adolescents with PBD are different from general shifts in mood experienced by children and adolescents because mood episodes last for long periods of time and cause severe disruptions to an individual's life. There are three known forms of PBD: Bipolar I, Bipolar II, and Bipolar Not Otherwise Specified (NOS). The average age of onset of PBD remains unclear, but reported age of onset ranges from 5 years of age to 19 years of age. PBD is typically more severe and has a poorer prognosis than bipolar disorder with onset in late-adolescence or adulthood.
The self-regulation of emotion or emotion regulation is the ability to respond to the ongoing demands of experience with the range of emotions in a manner that is socially tolerable and sufficiently flexible to permit spontaneous reactions as well as the ability to delay spontaneous reactions as needed. It can also be defined as extrinsic and intrinsic processes responsible for monitoring, evaluating, and modifying emotional reactions. The self-regulation of emotion belongs to the broader set of emotion regulation processes, which includes both the regulation of one's own feelings and the regulation of other people's feelings.
Prenatal stress, also known as prenatal maternal stress, occurs when an expectant mother is exposed to psychosocial or physical stress. This can be brought on by daily events or environmental hardships.[1] [2] According to the Developmental Origins of Health and Disease (DOHaD), a wide range of environmental factors a woman may experience during the perinatal period can contribute to biological impacts and changes in the fetus that then cause health risks later in the child's life. Health risks include impaired cognitive development, low birth weight, mental disorders, and gender specific deficits in the offspring.
Cyclothymia, also known as cyclothymic disorder, psychothemia / psychothymia, bipolar III, affective personality disorder and cyclothymic personality disorder, is a mental and behavioural disorder that involves numerous periods of symptoms of depression and periods of symptoms of elevated mood. These symptoms, however, are not sufficient to indicate a major depressive episode or a manic episode. Symptoms must last for more than one year in children and two years in adults.

Disruptive mood dysregulation disorder (DMDD) is a mental disorder in children and adolescents characterized by a persistently irritable or angry mood and frequent temper outbursts that are disproportionate to the situation and significantly more severe than the typical reaction of same-aged peers. DMDD was added to the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) as a type of mood disorder diagnosis for youths. The symptoms of DMDD resemble many other disorders, thus a differential includes attention deficit hyperactivity disorder (ADHD), oppositional defiant disorder (ODD), anxiety disorders, childhood bipolar disorder, intermittent explosive disorder (IED), major depressive disorder (MDD), and conduct disorder.
Interpersonal emotion regulation is the process of changing the emotional experience of one's self or another person through social interaction. It encompasses both intrinsic emotion regulation, in which one attempts to alter their own feelings by recruiting social resources, as well as extrinsic emotion regulation, in which one deliberately attempts to alter the trajectory of other people's feelings.
Emotional eating, also known as stress eating and emotional overeating, is defined as the "propensity to eat in response to positive and negative emotions". While the term commonly refers to eating as a means of coping with negative emotions, it sometimes includes eating for positive emotions, such as overeating when celebrating an event or to enhance an already good mood.

Emotions play a key role in overall mental health, and sleep plays a crucial role in maintaining the optimal homeostasis of emotional functioning. Deficient sleep, both in the form of sleep deprivation and restriction, adversely impacts emotion generation, emotion regulation, and emotional expression.
Borderline personality disorder (BPD) is a personality disorder characterized by a pervasive, long-term pattern of significant interpersonal relationship instability, a distorted sense of self, and intense emotional responses, which can be misdiagnosed. Misdiagnosis may involve erroneously assigning a BPD diagnosis to individuals not meeting the specific criteria or attributing an incorrect alternate diagnosis in cases where BPD is the accurate condition.
References
- 1 2 3 Acquired Brain Injury Outreach Service (2011). "Understanding Emotional Lability" (PDF). The State of Queensland (Queensland Health). Retrieved January 6, 2017.
- 1 2 Posner J, Kass E, Hulvershorn L (October 2014). "Using stimulants to treat ADHD-related emotional lability". Current Psychiatry Reports. 16 (10). Springer Nature: 478. doi:10.1007/s11920-014-0478-4. PMC 4243526 . PMID 25135778.
- ↑ Paris J (1993). Borderline Personality Disorder: Etiology and Treatment. American Psychiatric Pub. p. 106. ISBN 978-0-88048-408-4. OCLC 25281982.
- ↑ Kernberg OF (27 September 1995). Aggression in Personality Disorders and Perversions. Yale University Press. p. 58. ISBN 978-0-300-06508-4. OCLC 25965238.
- ↑ Schoenleber M, Berghoff CR, Gratz KL, Tull MT (January 2018). "Emotional lability and affective synchrony in posttraumatic stress disorder pathology". Journal of Anxiety Disorders. 53: 68–75. doi:10.1016/j.janxdis.2017.11.006. PMC 5748357 . PMID 29197703.
- ↑ Fortinash KM, Worret PA (13 June 2014). Psychiatric Mental Health Nursing. Elsevier Health Sciences. p. 230. ISBN 978-0-323-29327-3. OCLC 960964818.
- ↑ Kim JS (September 2016). "Post-stroke Mood and Emotional Disturbances: Pharmacological Therapy Based on Mechanisms". Journal of Stroke. 18 (3). Korean Stroke Society: 244–255. doi:10.5853/jos.2016.01144. PMC 5066431 . PMID 27733031.
- ↑ Cassara M (2002-08-20). "Hyperthyroidism" (PDF). Archived from the original (PDF) on 2018-07-23. Retrieved 2018-06-17.
- ↑ Stark MM, Payne-James JJ (30 April 2009). Symptoms and Signs of Substance Misuse. Cambridge University Press. p. 22. ISBN 978-0-521-13727-0. OCLC 656492372.
- ↑ Cooper RE, Tye C, Kuntsi J, Vassos E, Asherson P (January 2016). "The effect of omega-3 polyunsaturated fatty acid supplementation on emotional dysregulation, oppositional behaviour and conduct problems in ADHD: A systematic review and meta-analysis". Journal of Affective Disorders. 190. Elsevier BV: 474–482. doi:10.1016/j.jad.2015.09.053. PMID 26551407.
- 1 2 Maire J, Galéra C, Meyer E, Salla J, Michel G (May 2017). "Is emotional lability a marker for attention deficit hyperactivity disorder, anxiety and aggression symptoms in preschoolers?". Child and Adolescent Mental Health. 22 (2): 77–83. doi:10.1111/camh.12168. PMID 32680322. S2CID 148130518.
- ↑ Simonoff E, Jones CR, Pickles A, Happé F, Baird G, Charman T (November 2012). "Severe mood problems in adolescents with autism spectrum disorder". Journal of Child Psychology and Psychiatry, and Allied Disciplines. 53 (11): 1157–1166. doi:10.1111/j.1469-7610.2012.02600.x. PMID 22909395.
- ↑ Maguire SA, Williams B, Naughton AM, Cowley LE, Tempest V, Mann MK, et al. (September 2015). "A systematic review of the emotional, behavioural and cognitive features exhibited by school-aged children experiencing neglect or emotional abuse". Child. 41 (5). Wiley: 641–653. doi:10.1111/cch.12227. PMID 25733080.