Role in diagnosis
Thyroxine-binding globulin tests are sometimes used to find the cause of raised or lowered levels of thyroid hormone. This is done by measuring resin binding to labeled thyroid hormone, which happens only when the labeled thyroid hormone is free.
The patient's serum is mixed with the labeled thyroid hormone; next, the resin is added to the whole mixture to measure the amount of free labeled thyroid hormone. So, for instance, if the patient is truly hypothyroid, and TBG levels are normal, then there are many sites open for binding on the TBG, since the total thyroid hormone level is low. Therefore, when the labeled hormone is added, it will bind mostly to the TBG, leaving little of it left for binding to the resin. In contrast, however, if the patient is truly hyperthyroid, and TBG levels are normal, the patient's endogenous hormone will saturate the TBG binding sites more, leaving less room for the labeled hormone, which allows greater binding to the resin.
In patients who are truly hypo- or hyperthyroid, TBG testing is not very useful. However, if total thyroid hormone levels point to hypothyroidism or hyperthyroidism in the absence of accompanying symptoms, the utility of TBG testing becomes more evident, since TBG production can be modified by other factors such as estrogen levels, corticosteroid levels, or liver failure. If, for example, the TBG level is high, which can occur when estrogen levels are high, the TBG will bind more thyroid hormone, decreasing the free hormone available in the blood, which leads to stimulation of TSH, and the production of more thyroid hormone. In this case, the total thyroid hormone level will be high. And so, when labeled hormone is added, since TBG is so high, once equilibrium between the binding of endogenous thyroid hormone and the labeled hormone is achieved, less free labeled hormone will be available for uptake into the resin. On the converse, in the presence of corticosteroids, which lower TBG levels, the total thyroid hormone (bound and free) in the blood will be low. Thus, when the labeled hormone is added, since so little TBG is available in the blood, after equilibrium is achieved, only a small portion of it will bind, leaving plenty available for uptake by the resin.
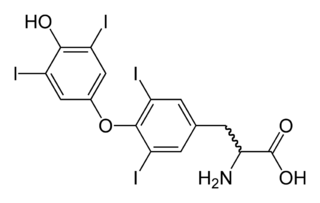
Hypothyroidism is a disorder of the endocrine system in which the thyroid gland does not produce enough thyroid hormones. It can cause a number of symptoms, such as poor ability to tolerate cold, extreme fatigue, muscle aches, constipation, slow heart rate, depression, and weight gain. Occasionally there may be swelling of the front part of the neck due to goitre. Untreated cases of hypothyroidism during pregnancy can lead to delays in growth and intellectual development in the baby or congenital iodine deficiency syndrome.

Iodothyronine deiodinases (EC 1.21.99.4 and EC 1.21.99.3) are a subfamily of deiodinase enzymes important in the activation and deactivation of thyroid hormones. Thyroxine (T4), the precursor of 3,5,3'-triiodothyronine (T3) is transformed into T3 by deiodinase activity. T3, through binding a nuclear thyroid hormone receptor, influences the expression of genes in practically every vertebrate cell. Iodothyronine deiodinases are unusual in that these enzymes contain selenium, in the form of an otherwise rare amino acid selenocysteine.
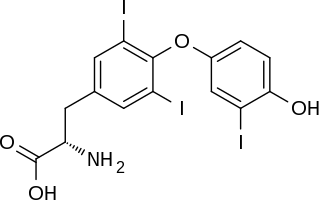
Triiodothyronine, also known as T3, is a thyroid hormone. It affects almost every physiological process in the body, including growth and development, metabolism, body temperature, and heart rate.

Transcortin, also known as corticosteroid-binding globulin (CBG) or serpin A6, is a protein produced in the liver in animals. In humans it is encoded by the SERPINA6 gene. It is an alpha-globulin.

Thyroid hormone resistance (also resistance to thyroid hormone (RTH), and sometimes Refetoff syndrome) describes a rare syndrome in which the thyroid hormone levels are elevated but the thyroid stimulating hormone (TSH) level is not suppressed, or not completely suppressed as would be expected. The first report of the condition appeared in 1967. Essentially this is decreased end organ responsiveness to thyroid hormones. A new term "impaired sensitivity to thyroid hormone" has been suggested in March 2014 by Refetoff et al.

Levothyroxine, also known as L-thyroxine, is a synthetic form of the thyroid hormone thyroxine (T4). It is used to treat thyroid hormone deficiency (hypothyroidism), including a severe form known as myxedema coma. It may also be used to treat and prevent certain types of thyroid tumors. It is not indicated for weight loss. Levothyroxine is taken orally (by mouth) or given by intravenous injection. Levothyroxine has a half-life of 7.5 days when taken daily, so about six weeks is required for it to reach a steady level in the blood.
Thyroid function tests (TFTs) is a collective term for blood tests used to check the function of the thyroid. TFTs may be requested if a patient is thought to suffer from hyperthyroidism or hypothyroidism, or to monitor the effectiveness of either thyroid-suppression or hormone replacement therapy. It is also requested routinely in conditions linked to thyroid disease, such as atrial fibrillation and anxiety disorder.
Desiccated thyroid, also known as thyroid extract, is thyroid gland that has been dried and powdered for medical use. It is used to treat hypothyroidism., but less preferred than levothyroxine. It is taken by mouth. Maximal effects may take up to three weeks to occur.

The hypothalamic–pituitary–thyroid axis is part of the neuroendocrine system responsible for the regulation of metabolism and also responds to stress.
Euthyroid sick syndrome (ESS) is a state of adaptation or dysregulation of thyrotropic feedback control wherein the levels of T3 and/or T4 are abnormal, but the thyroid gland does not appear to be dysfunctional. This condition may result from allostatic responses of hypothalamus-pituitary-thyroid feedback control, dyshomeostatic disorders, drug interferences, and impaired assay characteristics in critical illness.

Homeobox expressed in ES cells 1, also known as homeobox protein ANF, is a homeobox protein that in humans is encoded by the HESX1 gene.

Thyroid hormone receptor beta (TR-beta) also known as nuclear receptor subfamily 1, group A, member 2 (NR1A2), is a nuclear receptor protein that in humans is encoded by the THRB gene.

Homeobox protein prophet of PIT-1 is a protein that in humans is encoded by the PROP1 gene.

Mu-crystallin homolog also known as NADP-regulated thyroid-hormone-binding protein (THBP) is a protein that in humans is encoded by the CRYM gene. Multiple alternatively spliced transcript variants have been found for this gene.

Type II iodothyronine deiodinase is an enzyme that in humans is encoded by the DIO2 gene.

Thyroid hormones are any hormones produced and released by the thyroid gland, namely triiodothyronine (T3) and thyroxine (T4). They are tyrosine-based hormones that are primarily responsible for regulation of metabolism. T3 and T4 are partially composed of iodine, derived from food. A deficiency of iodine leads to decreased production of T3 and T4, enlarges the thyroid tissue and will cause the disease known as simple goitre.

Thyroid stimulating hormone, beta also known as TSHB is a protein which in humans is encoded by the TSHB gene.
Thyroid disease in pregnancy can affect the health of the mother as well as the child before and after delivery. Thyroid disorders are prevalent in women of child-bearing age and for this reason commonly present as a pre-existing disease in pregnancy, or after childbirth. Uncorrected thyroid dysfunction in pregnancy has adverse effects on fetal and maternal well-being. The deleterious effects of thyroid dysfunction can also extend beyond pregnancy and delivery to affect neurointellectual development in the early life of the child. Due to an increase in thyroxine binding globulin, an increase in placental type 3 deioidinase and the placental transfer of maternal thyroxine to the fetus, the demand for thyroid hormones is increased during pregnancy. The necessary increase in thyroid hormone production is facilitated by high human chorionic gonadotropin (hCG) concentrations, which bind the TSH receptor and stimulate the maternal thyroid to increase maternal thyroid hormone concentrations by roughly 50%. If the necessary increase in thyroid function cannot be met, this may cause a previously unnoticed (mild) thyroid disorder to worsen and become evident as gestational thyroid disease. Currently, there is not enough evidence to suggest that screening for thyroid dysfunction is beneficial, especially since treatment thyroid hormone supplementation may come with a risk of overtreatment. After women give birth, about 5% develop postpartum thyroiditis which can occur up to nine months afterwards. This is characterized by a short period of hyperthyroidism followed by a period of hypothyroidism; 20–40% remain permanently hypothyroid.
Thyroid hormone binding ratio (THBR) is a thyroid function test that measures the "uptake" of T3 or T4 tracer by thyroid-binding globulin (TBG) in a given serum sample. This provides an indirect and reciprocal estimate of the available binding sites on TBG within the sample.
The Thyrotroph Thyroid Hormone Sensitivity Index is a calculated structure parameter of thyroid homeostasis. It was originally developed to deliver a method for fast screening for resistance to thyroid hormone. Today it is also used to get an estimate for the set point of thyroid homeostasis, especially to assess dynamic thyrotropic adaptation of the anterior pituitary gland, including non-thyroidal illnesses.