
Coronary artery disease (CAD), also called coronary heart disease (CHD), ischemic heart disease (IHD), or simply heart disease, involves the reduction of blood flow to the heart muscle due to build-up of plaque (atherosclerosis) in the arteries of the heart. It is the most common of the cardiovascular diseases. Types include stable angina, unstable angina, myocardial infarction, and sudden cardiac death. A common symptom is chest pain or discomfort which may travel into the shoulder, arm, back, neck, or jaw. Occasionally it may feel like heartburn. Usually symptoms occur with exercise or emotional stress, last less than a few minutes, and improve with rest. Shortness of breath may also occur and sometimes no symptoms are present. In many cases, the first sign is a heart attack. Other complications include heart failure or an abnormal heartbeat.
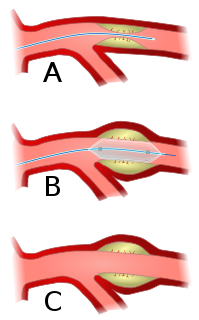
Angioplasty, also known as balloon angioplasty and percutaneous transluminal angioplasty (PTA), is a minimally invasive endovascular procedure used to widen narrowed or obstructed arteries or veins, typically to treat arterial atherosclerosis. A deflated balloon attached to a catheter is passed over a guide-wire into the narrowed vessel and then inflated to a fixed size. The balloon forces expansion of the blood vessel and the surrounding muscular wall, allowing an improved blood flow. A stent may be inserted at the time of ballooning to ensure the vessel remains open, and the balloon is then deflated and withdrawn. Angioplasty has come to include all manner of vascular interventions that are typically performed percutaneously.

Coronary artery bypass surgery, also known as coronary artery bypass graftsurgery, and colloquially heart bypass or bypass surgery, is a surgical procedure to restore normal blood flow to an obstructed coronary artery. A normal coronary artery transports blood to the heart muscle itself, not through the main circulatory system.

Peripheral artery disease (PAD) is an abnormal narrowing of arteries other than those that supply the heart or brain. When narrowing occurs in the heart, it is called coronary artery disease, and in the brain, it is called cerebrovascular disease. Peripheral artery disease most commonly affects the legs, but other arteries may also be involved – such as those of the arms, neck, or kidneys. The classic symptom is leg pain when walking which resolves with rest, known as intermittent claudication. Other symptoms include skin ulcers, bluish skin, cold skin, or abnormal nail and hair growth in the affected leg. Complications may include an infection or tissue death which may require amputation; coronary artery disease, or stroke. Up to 50% of people with PAD do not have symptoms.

Restenosis is the recurrence of stenosis, a narrowing of a blood vessel, leading to restricted blood flow. Restenosis usually pertains to an artery or other large blood vessel that has become narrowed, received treatment to clear the blockage and subsequently become renarrowed. This is usually restenosis of an artery, or other blood vessel, or possibly a vessel within an organ.

Percutaneous coronary intervention (PCI) is a procedure used to treat narrowing of the coronary arteries of the heart found in coronary artery disease. The process involves combining coronary angioplasty with stenting, which is the insertion of a permanent wire-meshed tube that is either drug eluting (DES) or composed of bare metal (BMS). The stent delivery balloon from the angioplasty catheter is inflated with media to force contact between the struts of the stent and the vessel wall, thus widening the blood vessel diameter. After accessing the blood stream through the femoral or radial artery, the procedure uses coronary catheterization to visualise the blood vessels on X-ray imaging. After this, an interventional cardiologist can perform a coronary angioplasty, using a balloon catheter in which a deflated balloon is advanced into the obstructed artery and inflated to relieve the narrowing; certain devices such as stents can be deployed to keep the blood vessel open. Various other procedures can also be performed.

A drug-eluting stent (DES) is a peripheral or coronary stent placed into narrowed, diseased peripheral or coronary arteries that slowly releases a drug to block cell proliferation. This prevents fibrosis that, together with clots (thrombi), could otherwise block the stented artery, a process called restenosis. The stent is usually placed within the peripheral or coronary artery by an interventional cardiologist or interventional radiologist during an angioplasty procedure.
The history of invasive and interventional cardiology is complex, with multiple groups working independently on similar technologies. Invasive and interventional cardiology is currently closely associated with cardiologists, though the development and most of its early research and procedures were performed by diagnostic and interventional radiologists.

Off-pump coronary artery bypass or "beating heart" surgery is a form of coronary artery bypass graft (CABG) surgery performed without cardiopulmonary bypass as a treatment for coronary heart disease. It was primarily developed in the early 1990s by Dr. Amano Atsushi. Historically, during bypass surgeries, the heart is stopped and a heart-lung machine takes over the work of the heart and lungs. When a cardiac surgeon chooses to perform the CABG procedure off-pump, also known as OPCAB, the heart is still beating while the graft attachments are made to bypass a blockage.

A coronary stent is a tube-shaped device placed in the coronary arteries that supply blood to the heart, to keep the arteries open in the treatment of coronary heart disease. It is used in a procedure called percutaneous coronary intervention (PCI). Coronary stents are now used in more than 90% of PCI procedures. Stents reduce angina and have been shown to improve survivability and decrease adverse events in an acute myocardial infarction.

Acute decompensated heart failure (ADHF) is a sudden worsening of the signs and symptoms of heart failure, which typically includes difficulty breathing (dyspnea), leg or feet swelling, and fatigue. ADHF is a common and potentially serious cause of acute respiratory distress. The condition is caused by severe congestion of multiple organs by fluid that is inadequately circulated by the failing heart. An attack of decompensation can be caused by underlying medical illness, such as myocardial infarction, an abnormal heart rhythm, infection, or thyroid disease.
Minimally invasive cardiac surgery, also known as MICS CABG or the McGinn technique is heart surgery performed through several small incisions instead of the traditional open-heart surgery that requires a median sternotomy approach. MICS CABG is a beating-heart multi-vessel procedure performed under direct vision through an anterolateral mini-thoracotomy.
Endoscopic vessel harvesting (EVH) is a surgical technique that may be used in conjunction with coronary artery bypass surgery. For patients with coronary artery disease, a physician may recommend a bypass to reroute blood around blocked arteries to restore and improve blood flow and oxygen to the heart. To create the bypass graft, a surgeon will remove or "harvest" healthy blood vessels from another part of the body, often from the patient's leg or arm. This vessel becomes a graft, with one end attaching to a blood source above and the other end below the blocked area, creating a "conduit" channel or new blood flow connection across the heart.

Reperfusion therapy is a medical treatment to restore blood flow, either through or around, blocked arteries, typically after a heart attack. Reperfusion therapy includes drugs and surgery. The drugs are thrombolytics and fibrinolytics used in a process called thrombolysis. Surgeries performed may be minimally-invasive endovascular procedures such as a percutaneous coronary intervention (PCI), followed by a coronary angioplasty. The angioplasty uses the insertion of a balloon to open up the artery, with the possible additional use of one or more stents. Other surgeries performed are the more invasive bypass surgeries that graft arteries around blockages.

Cardiac magnetic resonance imaging perfusion, also known as stress CMR perfusion, is a clinical magnetic resonance imaging test performed on patients with known or suspected coronary artery disease to determine if there are perfusion defects in the myocardium of the left ventricle that are caused by narrowing of one or more of the coronary arteries.
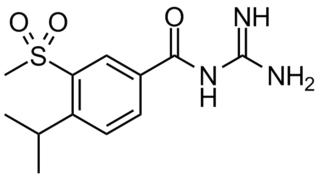
Cariporide is a selective Na+/H+ exchange inhibitor. Cariporide has been shown to actively suppress the cell death caused by oxidative stress.
A hybrid cardiac surgical procedure in a narrow sense is defined as a procedure that combines a conventional surgical part with an interventional part, using some sort of catheter-based procedure guided by fluoroscopy imaging in a hybrid OR without interruption. A wider definition includes a clinically connected succession of a catheter intervention and a surgical procedure with a time gap.
Inclacumab (LC1004-002) (INN) is a human monoclonal antibody designed for the treatment of cardiovascular disease.
Remote ischemic conditioning (RIC) is an experimental medical procedure that aims to reduce the severity of ischaemic injury to an organ such as the heart or the brain, most commonly in the situation of a heart attack or a stroke, or during procedures such as heart surgery when the heart may temporary suffer ischaemia during the operation, by triggering the body's natural protection against tissue injury. Although noted to have some benefits in experimental models in animals, this is still an experimental procedure in humans and initial evidence from small studies have not been replicated in larger clinical trials. Successive clinical trials have failed to identify evidence supporting a protective role in humans.
In medicine, vein graft failure (VGF) is a condition in which vein grafts, which are used as alternative conduits in bypass surgeries, get occluded.











