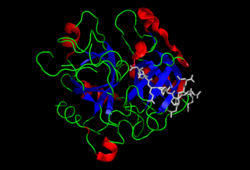
1a2c: STRUCTURE OF THROMBIN INHIBITED BY AERUGINOSIN298-A FROM A BLUE-GREEN ALGA
1a3b: COMPLEX OF HUMAN ALPHA-THROMBIN WITH THE BIFUNCTIONAL BORONATE INHIBITOR BOROLOG1
1a3e: COMPLEX OF HUMAN ALPHA-THROMBIN WITH THE BIFUNCTIONAL BORONATE INHIBITOR BOROLOG2
1a46: THROMBIN COMPLEXED WITH HIRUGEN AND A BETA-STRAND MIMETIC INHIBITOR
1a4w: CRYSTAL STRUCTURES OF THROMBIN WITH THIAZOLE-CONTAINING INHIBITORS: PROBES OF THE S1' BINDING SITE
1a5g: HUMAN THROMBIN COMPLEXED WITH NOVEL SYNTHETIC PEPTIDE MIMETIC INHIBITOR AND HIRUGEN
1a61: THROMBIN COMPLEXED WITH A BETA-MIMETIC THIAZOLE-CONTAINING INHIBITOR
1abi: STRUCTURE OF THE HIRULOG 3-THROMBIN COMPLEX AND NATURE OF THE S' SUBSITES OF SUBSTRATES AND INHIBITORS
1abj: STRUCTURE OF THE HIRULOG 3-THROMBIN COMPLEX AND NATURE OF THE S' SUBSITES OF SUBSTRATES AND INHIBITORS
1ad8: COMPLEX OF THROMBIN WITH AND INHIBITOR CONTAINING A NOVEL P1 MOIETY
1ae8: HUMAN ALPHA-THROMBIN INHIBITION BY EOC-D-PHE-PRO-AZALYS-ONP
1aht: CRYSTAL STRUCTURE OF HUMAN ALPHA-THROMBIN COMPLEXED WITH HIRUGEN AND P-AMIDINOPHENYLPYRUVATE) AT 1.6 ANGSTROMS RESOLUTION
1ai8: HUMAN ALPHA-THROMBIN TERNARY COMPLEX WITH THE EXOSITE INHIBITOR HIRUGEN AND ACTIVE SITE INHIBITOR PHCH2OCO-D-DPA-PRO-BOROMPG
1aix: HUMAN ALPHA-THROMBIN TERNARY COMPLEX WITH EXOSITE INHIBITOR HIRUGEN AND ACTIVE SITE INHIBITOR PHCH2OCO-D-DPA-PRO-BOROVAL
1awf: NOVEL COVALENT THROMBIN INHIBITOR FROM PLANT EXTRACT
1awh: NOVEL COVALENT THROMBIN INHIBITOR FROM PLANT EXTRACT
1ay6: THROMBIN INHIBITOR FROM THEONALLA, CYCLOTHEANAMIDE-BASED MACROCYCLIC TRIPEPTIDE MOTIF
1b5g: HUMAN THROMBIN COMPLEXED WITH NOVEL SYNTHETIC PEPTIDE MIMETIC INHIBITOR AND HIRUGEN
1b7x: STRUCTURE OF HUMAN ALPHA-THROMBIN Y225I MUTANT BOUND TO D-PHE-PRO-ARG-CHLOROMETHYLKETONE
1ba8: THROMBIN INHIBITOR WITH A RIGID TRIPEPTIDYL ALDEHYDES
1bb0: THROMBIN INHIBITORS WITH RIGID TRIPEPTIDYL ALDEHYDES
1bbr: THE STRUCTURE OF RESIDUES 7-16 OF THE A ALPHA CHAIN OF HUMAN FIBRINOGEN BOUND TO BOVINE THROMBIN AT 2.3 ANGSTROMS RESOLUTION
1bcu: ALPHA-THROMBIN COMPLEXED WITH HIRUGEN AND PROFLAVIN
1bhx: X-RAY STRUCTURE OF THE COMPLEX OF HUMAN ALPHA THROMBIN WITH THE INHIBITOR SDZ 229-357
1bth: STRUCTURE OF THROMBIN COMPLEXED WITH BOVINE PANCREATIC TRYPSIN INHIBITOR
1c1u: RECRUITING ZINC TO MEDIATE POTENT, SPECIFIC INHIBITION OF SERINE PROTEASES
1c1v: RECRUITING ZINC TO MEDIATE POTENT, SPECIFIC INHIBITION OF SERINE PROTEASES
1c1w: RECRUITING ZINC TO MEDIATE POTENT, SPECIFIC INHIBITION OF SERINE PROTEASES
1c4u: SELECTIVE NON ELECTROPHILIC THROMBIN INHIBITORS WITH CYCLOHEXYL MOIETIES.
1c4v: SELECTIVE NON ELECTROPHILIC THROMBIN INHIBITORS WITH CYCLOHEXYL MOIETIES.
1c4y: SELECTIVE NON-ELECTROPHILIC THROMBIN INHIBITORS
1c5l: STRUCTURAL BASIS FOR SELECTIVITY OF A SMALL MOLECULE, S1-BINDING, SUB-MICROMOLAR INHIBITOR OF UROKINASE TYPE PLASMINOGEN ACTIVATOR
1c5n: STRUCTURAL BASIS FOR SELECTIVITY OF A SMALL MOLECULE, S1-BINDING, SUB-MICROMOLAR INHIBITOR OF UROKINASE TYPE PLASMINOGEN ACTIVATOR
1c5o: STRUCTURAL BASIS FOR SELECTIVITY OF A SMALL MOLECULE, S1-BINDING, SUB-MICROMOLAR INHIBITOR OF UROKINASE TYPE PLASMINOGEN ACTIVATOR
1ca8: THROMBIN INHIBITORS WITH RIGID TRIPEPTIDYL ALDEHYDES
1d3d: CRYSTAL STRUCTURE OF HUMAN ALPHA THROMBIN IN COMPLEX WITH BENZOTHIOPHENE INHIBITOR 4
1d3p: CRYSTAL STRUCTURE OF HUMAN ALPHA-THROMBIN IN COMPLEX WITH BENZO[B]THIOPHENE INHIBITOR 3
1d3q: CRYSTAL STRUCTURE OF HUMAN ALPHA THROMBIN IN COMPLEX WITH BENZO[B]THIOPHENE INHIBITOR 2
1d3t: CRYSTAL STRUCTURE OF HUMAN ALPHA THROMBIN IN COMPLEX WITH BENZO[B]THIOPHENE INHIBITOR 1
1d4p: CRYSTAL STRUCTURE OF HUMAN ALPHA THROMBIN IN COMPLEX WITH 5-AMIDINOINDOLE-4-BENZYLPIPERIDINE INHIBITOR
1d6w: STRUCTURE OF THROMBIN COMPLEXED WITH SELECTIVE NON-ELECTROPHILIC INHIBITORS HAVING CYCLOHEXYL MOIETIES AT P1
1d9i: STRUCTURE OF THROMBIN COMPLEXED WITH SELECTIVE NON-ELECTOPHILIC INHIBITORS HAVING CYCLOHEXYL MOIETIES AT P1
1de7: INTERACTION OF FACTOR XIII ACTIVATION PEPTIDE WITH ALPHA-THROMBIN: CRYSTAL STRUCTURE OF THE ENZYME-SUBSTRATE COMPLEX
1dit: COMPLEX OF A DIVALENT INHIBITOR WITH THROMBIN
1dm4: SER195ALA MUTANT OF HUMAN THROMBIN COMPLEXED WITH FIBRINOPEPTIDE A (7-16)
1doj: Crystal structure of human alpha-thrombin*RWJ-51438 complex at 1.7 A
1dwb: CRYSTALLOGRAPHIC ANALYSIS AT 3.0-ANGSTROMS RESOLUTION OF THE BINDING TO HUMAN THROMBIN OF FOUR ACTIVE SITE-DIRECTED INHIBITORS
1dwc: CRYSTALLOGRAPHIC ANALYSIS AT 3.0-ANGSTROMS RESOLUTION OF THE BINDING TO HUMAN THROMBIN OF FOUR ACTIVE SITE-DIRECTED INHIBITORS
1dwd: CRYSTALLOGRAPHIC ANALYSIS AT 3.0-ANGSTROMS RESOLUTION OF THE BINDING TO HUMAN THROMBIN OF FOUR ACTIVE SITE-DIRECTED INHIBITORS
1dwe: CRYSTALLOGRAPHIC ANALYSIS AT 3.0-ANGSTROMS RESOLUTION OF THE BINDING TO HUMAN THROMBIN OF FOUR ACTIVE SITE-DIRECTED INHIBITORS
1dx5: CRYSTAL STRUCTURE OF THE THROMBIN-THROMBOMODULIN COMPLEX
1e0f: CRYSTAL STRUCTURE OF THE HUMAN ALPHA-THROMBIN-HAEMADIN COMPLEX: AN EXOSITE II-BINDING INHIBITOR
1eb1: COMPLEX STRUCTURE OF HUMAN THROMBIN WITH N-METHYL-ARGININE INHIBITOR
1eoj: DESIGN OF P1' AND P3' RESIDUES OF TRIVALENT THROMBIN INHIBITORS AND THEIR CRYSTAL STRUCTURES
1eol: DESIGN OF P1' AND P3' RESIDUES OF TRIVALENT THROMBIN INHIBITORS AND THEIR CRYSTAL STRUCTURES
1fpc: ACTIVE SITE MIMETIC INHIBITION OF THROMBIN
1fph: THE INTERACTION OF THROMBIN WITH FIBRINOGEN: A STRUCTURAL BASIS FOR ITS SPECIFICITY
1g30: THROMBIN INHIBITOR COMPLEX
1g32: THROMBIN INHIBITOR COMPLEX
1g37: CRYSTAL STRUCTURE OF HUMAN ALPHA-THROMBIN COMPLEXED WITH BCH-10556 AND EXOSITE-DIRECTED PEPTIDE
1ghv: A NOVEL SERINE PROTEASE INHIBITION MOTIF INVOLVING A MULTI-CENTERED SHORT HYDROGEN BONDING NETWORK AT THE ACTIVE SITE
1ghw: A NOVEL SERINE PROTEASE INHIBITION MOTIF INVOLVING A MULTI-CENTERED SHORT HYDROGEN BONDING NETWORK AT THE ACTIVE SITE
1ghx: A NOVEL SERINE PROTEASE INHIBITION MOTIF INVOLVING A MULTI-CENTERED SHORT HYDROGEN BONDING NETWORK AT THE ACTIVE SITE
1ghy: A NOVEL SERINE PROTEASE INHIBITION MOTIF INVOLVING A MULTI-CENTERED SHORT HYDROGEN BONDING NETWORK AT THE ACTIVE SITE
1gj4: SELECTIVITY AT S1, H2O DISPLACEMENT, UPA, TPA, SER190/ALA190 PROTEASE, STRUCTURE-BASED DRUG DESIGN
1gj5: SELECTIVITY AT S1, H2O DISPLACEMENT, UPA, TPA, SER190/ALA190 PROTEASE, STRUCTURE-BASED DRUG DESIGN
1h8d: X-RAY STRUCTURE OF THE HUMAN ALPHA-THROMBIN COMPLEX WITH A TRIPEPTIDE PHOSPHONATE INHIBITOR.
1h8i: X-RAY CRYSTAL STRUCTURE OF HUMAN ALPHA-THROMBIN WITH A TRIPEPTIDE PHOSPHONATE INHIBITOR.
1hag: THE ISOMORPHOUS STRUCTURES OF PRETHROMBIN2, HIRUGEN-AND PPACK-THROMBIN: CHANGES ACCOMPANYING ACTIVATION AND EXOSITE BINDING TO THROMBIN
1hah: THE ISOMORPHOUS STRUCTURES OF PRETHROMBIN2, HIRUGEN-AND PPACK-THROMBIN: CHANGES ACCOMPANYING ACTIVATION AND EXOSITE BINDING TO THROMBIN
1hai: THE ISOMORPHOUS STRUCTURES OF PRETHROMBIN2, HIRUGEN-AND PPACK-THROMBIN: CHANGES ACCOMPANYING ACTIVATION AND EXOSITE BINDING TO THROMBIN
1hao: COMPLEX OF HUMAN ALPHA-THROMBIN WITH A 15MER OLIGONUCLEOTIDE GGTTGGTGTGGTTGG (BASED ON NMR MODEL OF DNA
1hap: COMPLEX OF HUMAN ALPHA-THROMBIN WITH A 15MER OLIGONUCLEOTIDE GGTTGGTGTGGTTGG (BASED ON X-RAY MODEL OF DNA)
1hbt: HUMAN ALPHA-THROMBIN COMPLEXED WITH A PEPTIDYL PYRIDINIUM METHYL KETONE CONTAINING BIVALENT INHIBITOR
1hdt: STRUCTURE OF A RETRO-BINDING PEPTIDE INHIBITOR COMPLEXED WITH HUMAN ALPHA-THROMBIN
1hgt: STRUCTURE OF THE HIRUGEN AND HIRULOG 1 COMPLEXES OF ALPHA-THROMBIN
1hlt: THE STRUCTURE OF A NONADECAPEPTIDE OF THE FIFTH EGF DOMAIN OF THROMBOMODULIN COMPLEXED WITH THROMBIN
1hut: THE STRUCTURE OF ALPHA-THROMBIN INHIBITED BY A 15-MER SINGLE-STRANDED DNA APTAMER
1hxe: SERINE PROTEASE
1hxf: HUMAN THROMBIN COMPLEX WITH HIRUDIN VARIANT
1ihs: CRYSTAL STRUCTURE OF THE COMPLEX OF HUMAN ALPHA-THROMBIN AND NON-HYDROLYZABLE BIFUNCTIONAL INHIBITORS, HIRUTONIN-2 AND HIRUTONIN-6
1iht: CRYSTAL STRUCTURE OF THE COMPLEX OF HUMAN ALPHA-THROMBIN AND NON-HYDROLYZABLE BIFUNCTIONAL INHIBITORS, HIRUTONIN-2 AND HIRUTONIN-6
1jmo: Crystal Structure of the Heparin Cofactor II-S195A Thrombin Complex
1jou: Crystal Structure of Native S195A Thrombin with an Unoccupied Active Site
1jwt: CRYSTAL STRUCTURE OF THROMBIN IN COMPLEX WITH A NOVEL BICYCLIC LACTAM INHIBITOR
1k21: HUMAN THROMBIN-INHIBITOR COMPLEX
1k22: HUMAN THROMBIN-INHIBITOR COMPLEX
1kts: Thrombin Inhibitor Complex
1ktt: Thrombin inhibitor complex
1lhc: HUMAN ALPHA-THROMBIN COMPLEXED WITH AC-(D)PHE-PRO-BOROARG-OH
1lhd: HUMAN ALPHA-THROMBIN COMPLEXED WITH AC-(D)PHE-PRO-BOROLYS-OH
1lhe: HUMAN ALPHA-THROMBIN COMPLEXED WITH AC-(D)PHE-PRO-BORO-N-BUTYL-AMIDINO-GLYCINE-OH
1lhf: HUMAN ALPHA-THROMBIN COMPLEXED WITH AC-(D)PHE-PRO-BORO-HOMOLYS-OH
1lhg: HUMAN ALPHA-THROMBIN COMPLEXED WITH AC-(D)PHE-PRO-BOROORNITHINE-OH
1mh0: Crystal structure of the anticoagulant slow form of thrombin
1mu6: Crystal Structure of Thrombin in Complex with L-378,622
1mu8: thrombin-hirugen_l-378,650
1mue: Thrombin-Hirugen-L405,426
1nm6: thrombin in complex with selective macrocyclic inhibitor at 1.8A
1no9: Design of weakly basic thrombin inhibitors incorporating novel P1 binding functions: molecular and X-ray crystallographic studies.
1nrn: CRYSTALLOGRAPHIC STRUCTURES OF THROMBIN COMPLEXED WITH THROMBIN RECEPTOR PEPTIDES: EXISTENCE OF EXPECTED AND NOVEL BINDING MODES
1nro: CRYSTALLOGRAPHIC STRUCTURES OF THROMBIN COMPLEXED WITH THROMBIN RECEPTOR PEPTIDES: EXISTENCE OF EXPECTED AND NOVEL BINDING MODES
1nrp: CRYSTALLOGRAPHIC STRUCTURES OF THROMBIN COMPLEXED WITH THROMBIN RECEPTOR PEPTIDES: EXISTENCE OF EXPECTED AND NOVEL BINDING MODES
1nrq: CRYSTALLOGRAPHIC STRUCTURES OF THROMBIN COMPLEXED WITH THROMBIN RECEPTOR PEPTIDES: EXISTENCE OF EXPECTED AND NOVEL BINDING MODES
1nrr: CRYSTALLOGRAPHIC STRUCTURES OF THROMBIN COMPLEXED WITH THROMBIN RECEPTOR PEPTIDES: EXISTENCE OF EXPECTED AND NOVEL BINDING MODES
1nrs: CRYSTALLOGRAPHIC STRUCTURES OF THROMBIN COMPLEXED WITH THROMBIN RECEPTOR PEPTIDES: EXISTENCE OF EXPECTED AND NOVEL BINDING MODES
1nt1: thrombin in complex with selective macrocyclic inhibitor
1nu7: Staphylocoagulase-Thrombin Complex
1nu9: Staphylocoagulase-Prethrombin-2 complex
1ny2: Human alpha thrombin inhibited by RPPGF and hirugen
1nzq: D-Phe-Pro-Arg-Type Thrombin Inhibitor
1o0d: Human Thrombin complexed with a d-Phe-Pro-Arg-type Inhibitor and a C-terminal Hirudin derived exo-site inhibitor
1o2g: Elaborate Manifold of Short Hydrogen Bond Arrays Mediating Binding of Active Site-Directed Serine Protease Inhibitors
1o5g: Dissecting and Designing Inhibitor Selectivity Determinants at the S1 site Using an Artificial Ala190 Protease (Ala190 uPA)
1ook: Crystal Structure of the Complex of Platelet Receptor GPIb-alpha and Human alpha-Thrombin
1oyt: COMPLEX OF RECOMBINANT HUMAN THROMBIN WITH A DESIGNED FLUORINATED INHIBITOR
1p8v: CRYSTAL STRUCTURE OF THE COMPLEX OF PLATELET RECEPTOR GPIB-ALPHA AND ALPHA-THROMBIN AT 2.6A
1ppb: THE REFINED 1.9 ANGSTROMS CRYSTAL STRUCTURE OF HUMAN ALPHA-THROMBIN: INTERACTION WITH D-PHE-PRO-ARG CHLOROMETHYLKETONE AND SIGNIFICANCE OF THE TYR-PRO-PRO-TRP INSERTION SEGMENT
1qbv: CRYSTAL STRUCTURE OF THROMBIN COMPLEXED WITH AN GUANIDINE-MIMETIC INHIBITOR
1qhr: NOVEL COVALENT ACTIVE SITE THROMBIN INHIBITORS
1qj1: NOVEL COVALENT ACTIVE SITE THROMBIN INHIBITORS
1qj6: NOVEL COVALENT ACTIVE SITE THROMBIN INHIBITORS
1qj7: NOVEL COVALENT ACTIVE SITE THROMBIN INHIBITORS
1qur: HUMAN ALPHA-THROMBIN IN COMPLEX WITH BIVALENT, BENZAMIDINE-BASED SYNTHETIC INHIBITOR
1rd3: 2.5A Structure of Anticoagulant Thrombin Variant E217K
1riw: Thrombin in complex with natural product inhibitor Oscillarin
1sb1: Novel Non-Covalent Thrombin Inhibitors Incorporating P1 4,5,6,7-Tetrahydrobenzothiazole Arginine Side Chain Mimetics
1sfq: Fast form of thrombin mutant R(77a)A bound to PPACK
1sgi: Crystal structure of the anticoagulant slow form of thrombin
1shh: Slow form of Thrombin Bound with PPACK
1sl3: crystal structure of Thrombin in complex with a potent P1 heterocycle-Aryl based inhibitor
1sr5: ANTITHROMBIN-ANHYDROTHROMBIN-HEPARIN TERNARY COMPLEX STRUCTURE
1t4u: Crystal Structure Analysis of a novel Oxyguanidine bound to Thrombin
1t4v: Crystal Structure Analysis of a novel Oxyguanidine bound to Thrombin
1ta2: Crystal structure of thrombin in complex with compound 1
1ta6: Crystal structure of thrombin in complex with compound 14b
1tb6: 2.5A Crystal Structure of the Antithrombin-Thrombin-Heparin Ternary Complex
1tbz: HUMAN THROMBIN WITH ACTIVE SITE N-METHYL-D PHENYLALANYL-N-[5-(AMINOIMINOMETHYL)AMINO]-1-[(BENZOTHIAZOLYL)CARBONYL] BUTYL]-L-PROLINAMIDE TRIFLUROACETATE AND EXOSITE-HIRUGEN
1thp: STRUCTURE OF HUMAN ALPHA-THROMBIN Y225P MUTANT BOUND TO D-PHE-PRO-ARG-CHLOROMETHYLKETONE
1thr: STRUCTURES OF THROMBIN COMPLEXES WITH A DESIGNED AND A NATURAL EXOSITE INHIBITOR
1ths: STRUCTURES OF THROMBIN COMPLEXES WITH A DESIGNED AND A NATURAL EXOSITE INHIBITOR
1tmb: MOLECULAR BASIS FOR THE INHIBITION OF HUMAN ALPHA-THROMBIN BY THE MACROCYCLIC PEPTIDE CYCLOTHEONAMIDE A
1tmt: CHANGES IN INTERACTIONS IN COMPLEXES OF HIRUDIN DERIVATIVES AND HUMAN ALPHA-THROMBIN DUE TO DIFFERENT CRYSTAL FORMS
1tmu: CHANGES IN INTERACTIONS IN COMPLEXES OF HIRUDIN DERIVATIVES AND HUMAN ALPHA-THROMBIN DUE TO DIFFERENT CRYSTAL FORMS
1tom: ALPHA-THROMBIN COMPLEXED WITH HIRUGEN
1tq0: Crystal structure of the potent anticoagulant thrombin mutant W215A/E217A in free form
1tq7: Crystal structure of the anticoagulant thrombin mutant W215A/E217A bound to PPACK
1twx: Crystal structure of the thrombin mutant D221A/D222K
1ucy: THROMBIN COMPLEXED WITH FIBRINOPEPTIDE A ALPHA (RESIDUES 7-19). THREE COMPLEXES, ONE WITH EPSILON-THROMBIN AND TWO WITH ALPHA-THROMBIN
1uma: ALPHA-THROMBIN (HIRUGEN) COMPLEXED WITH NA-(N,N-DIMETHYLCARBAMOYL)-ALPHA-AZALYSINE
1uvs: BOVINE THROMBIN--BM51.1011 COMPLEX
1vit: THROMBIN:HIRUDIN 51-65 COMPLEX
1vr1: Specificity for Plasminogen Activator Inhibitor-1
1vzq: COMPLEX OF THROMBIN WITH DESIGNED INHIBITOR 7165
1w7g: ALPHA-THROMBIN COMPLEX WITH SULFATED HIRUDIN (RESIDUES 54-65) AND L-ARGININE TEMPLATE INHIBITOR CS107
1way: ACTIVE SITE THROMBIN INHIBITORS
1wbg: ACTIVE SITE THROMBIN INHIBITORS
1xm1: Nonbasic Thrombin Inhibitor Complex
1xmn: Crystal structure of thrombin bound to heparin
1ycp: THE CRYSTAL STRUCTURE OF FIBRINOGEN-AA PEPTIDE 1-23 (F8Y) BOUND TO BOVINE THROMBIN EXPLAINS WHY THE MUTATION OF PHE-8 TO TYROSINE STRONGLY INHIBITS NORMAL CLEAVAGE AT ARGININE-16
1ype: Thrombin Inhibitor Complex
1ypg: Thrombin Inhibitor Complex
1ypj: Thrombin Inhibitor Complex
1ypk: Thrombin Inhibitor Complex
1ypl: X-ray crystal structure of thrombin inhibited by synthetic cyanopeptide analogue RA-1008
1ypm: X-ray crystal structure of thrombin inhibited by synthetic cyanopeptide analogue RA-1014
1z71: thrombin and P2 pyridine N-oxide inhibitor complex structure
1z8i: Crystal structure of the thrombin mutant G193A bound to PPACK
1z8j: Crystal structure of the thrombin mutant G193P bound to PPACK
1zgi: thrombin in complex with an oxazolopyridine inhibitor 21
1zgv: Thrombin in complex with an oxazolopyridine inhibitor 2
1zrb: Thrombin in complex with an azafluorenyl inhibitor 23b
2a0q: Structure of thrombin in 400 mM potassium chloride
2a2x: Orally Active Thrombin Inhibitors in Complex with Thrombin Inh12
2a45: Crystal structure of the complex between thrombin and the central ""E"" region of fibrin
2afq: 1.9 angstrom crytal structure of wild-type human thrombin in the sodium free state
2ank: orally active thrombin inhibitors in complex with thrombin and an exosite decapeptide
2anm: Ternary complex of an orally active thrombin inhibitor with human thrombin and a c-terminal hirudin derived exo-sit inhibitor
2b5t: 2.1 Angstrom structure of a nonproductive complex between antithrombin, synthetic heparin mimetic SR123781 and two S195A thrombin molecules
2bdy: thrombin in complex with inhibitor
2bvr: HUMAN THROMBIN COMPLEXED WITH FRAGMENT-BASED SMALL MOLECULES OCCUPYING THE S1 POCKET
2bvs: HUMAN THROMBIN COMPLEXED WITH FRAGMENT-BASED SMALL MOLECULES OCCUPYING THE S1 POCKET
2bvx: DESIGN AND DISCOVERY OF NOVEL, POTENT THROMBIN INHIBITORS WITH A SOLUBILIZING CATIONIC P1-P2-LINKER
2bxt: DESIGN AND DISCOVERY OF NOVEL, POTENT THROMBIN INHIBITORS WITH A SOLUBILIZING CATIONIC P1-P2-LINKER
2bxu: DESIGN AND DISCOVERY OF NOVEL, POTENT THROMBIN INHIBITORS WITH A SOLUBILIZING CATIONIC P1-P2-LINKER
2c8w: THROMBIN INHIBITORS
2c8x: THROMBIN INHIBITORS
2c8y: THROMBIN INHIBITORS
2c8z: THROMBIN INHIBITORS
2c90: THROMBIN INHIBITORS
2c93: THROMBIN INHIBITORS
2cf8: COMPLEX OF RECOMBINANT HUMAN THROMBIN WITH A INHIBITOR
2cf9: COMPLEX OF RECOMBINANT HUMAN THROMBIN WITH A INHIBITOR
2cn0: COMPLEX OF RECOMBINANT HUMAN THROMBIN WITH A DESIGNED INHIBITOR
2feq: orally active thrombin inhibitors
2fes: Orally active thrombin inhibitors
2gde: Thrombin in complex with inhibitor
2gp9: Crystal structure of the slow form of thrombin in a self-inhibited conformation
2h9t: Crystal structure of human alpha-thrombin in complex with suramin
2hgt: STRUCTURE OF THE HIRUGEN AND HIRULOG 1 COMPLEXES OF ALPHA-THROMBIN
2hnt: CRYSTALLOGRAPHIC STRUCTURE OF HUMAN GAMMA-THROMBIN
2hpp: STRUCTURES OF THE NONCOVALENT COMPLEXES OF HUMAN AND BOVINE PROTHROMBIN FRAGMENT 2 WITH HUMAN PPACK-THROMBIN
2hpq: STRUCTURES OF THE NONCOVALENT COMPLEXES OF HUMAN AND BOVINE PROTHROMBIN FRAGMENT 2 WITH HUMAN PPACK-THROMBIN
2hwl: Crystal structure of thrombin in complex with fibrinogen gamma' peptide
2jh0: HUMAN THROMBIN HIRUGEN INHIBITOR COMPLEX.
2jh5: HUMAN THROMBIN HIRUGEN INHIBITOR COMPLEX.
2jh6: HUMAN THROMBIN HIRUGEN INHIBITOR COMPLEX.
2od3: Human thrombin chimera with human residues 184a, 186, 186a, 186b, 186c and 222 replaced by murine thrombin equivalents.
2thf: STRUCTURE OF HUMAN ALPHA-THROMBIN Y225F MUTANT BOUND TO D-PHE-PRO-ARG-CHLOROMETHYLKETONE
3hat: ACTIVE SITE MIMETIC INHIBITION OF THROMBIN
4htc: THE REFINED STRUCTURE OF THE HIRUDIN-THROMBIN COMPLEX
4thn: THE CRYSTAL STRUCTURE OF ALPHA-THROMBIN-HIRUNORM IV COMPLEX REVEALS A NOVEL SPECIFICITY SITE RECOGNITION MODE.
5gds: HIRUNORMS ARE TRUE HIRUDIN MIMETICS. THE CRYSTAL STRUCTURE OF HUMAN ALPHA-THROMBIN:HIRUNORM V COMPLEX
7kme: CRYSTAL STRUCTURE OF HUMAN ALPHA-THROMBIN INHIBITED WITH SEL2711.
8kme: CRYSTAL STRUCTURE OF HUMAN ALPHA-THROMBIN INHIBITED WITH SEL2770.